

This third issue of GaBI Journal is the last of the volume for this year and marks the end of the first year of me taking up the Editor-in-Chief position for the journal. We have seen a very considerable variety of papers submitted and published during 2024.
The first Review Article in this issue by Dr Shivani Mittra et al. is titled ‘Aligning environmental, social, and governance to clinical development: moving towards more sustainable clinical trials’. These authors point out that drug development is among the highest producers of greenhouse gas emissions with clinical trials being the main culprit. They consider that there is an urgent requirement to develop tools capable of measuring the carbon footprint of clinical trials and guidelines on how to reduce it. The comprehensive article discusses how regulators, pharmaceutical companies, and clinical researchers can align with the environmental, social, and governance goals for the efficient conduct of clinical trials, including those for biologicals and biosimilars.
The issue continues with the second Review Article of international initiatives on pharmaceutical regulatory reliance and recognition by Mr Vimal Sachdeva of the World Heath Organization (WHO). This brightly illustrated contribution emphasises the pressure on organizations like WHO to facilitate timely access to safe, effective, and good-quality health products worldwide. It highlights the need to harmonize regulatory decisions and expedite the regulatory approval process.
This is followed by a Perspective by Drs Joseph P Park and Gillian R Woollett titled ‘US interchangeability designation: are we ready to cut the Gordian knot?’ It discusses how the US Food and Drug Administration’s current thinking on interchangeability has evolved since the legal designation was first created some time ago and strongly supports the improvements implemented. This is a continuation of publications by these authors on this and similar issues.
The next article is a Perspective titled ‘The challenge for drug shortage: lessons learned from the quality issues of Japanese generic drug companies’ from Dr Takanao Hashimoto et al. This examines the repercussions of recent quality and regulatory crises in Japan’s generic pharmaceutical sector, focusing on incidents involving Sawai Group Holdings and other manufacturers. It calls for strategic reforms to reconcile cost containment with quality and supply chain stability, ensuring the pharmaceutical industry can meet both domestic and international healthcare demands effectively.
The final item in this issue is a sponsor-funded editorial summarizing an interview on ‘Transforming healthcare: CinnaGen’s leadership in follow-on biologicals/biosimilars development and market expansion’ with Dr Haleh Hamedifar who is the Chairperson of CinnaGen. CinnaGen is the largest Iranian biopharmaceutical company and the biggest such company in the Middle East and North Africa (MENA) region. Its commitment to affordable, accessible health care through the development of high-quality follow-on products is transforming patient care, particularly in underserved regions like MENA.
I wish all readers and contributors of GaBI Journal the very best for 2025.
Robin Thorpe, PhD., FRCPath
Editor-in-Chief, GaBIJournal
Disclosure of Conflict of Interest Statement is available upon request.
Copyright © 2024 Pro Pharma Communications International
Permission granted to reproduce for personal and non-commercial use only. All other reproduction, copy or reprinting of all or part of any ‘Content’ found on this website is strictly prohibited without the prior consent of the publisher. Contact the publisher to obtain permission before redistributing.
Source URL: https://gabi-journal.net/third-and-final-issue-of-gabi-journals-13th-volume.html
Issue 2 of Volume 13 of GaBI Journal starts with a Review Article by Paul et al., titled ‘Increasing adoption of quality-assured biosimilars to address access challenges in low- and middle-income countries’. The review focuses on treatment of non-communicable diseases as these disproportionately affect people living in low- and middle-income countries compared to high-income countries. Challenges identified include weaker regulatory frameworks, dependence on importation, low awareness of biosimilars, and the need for effective policies encouraging access to and use of biosimilars. The review identifies additional criteria, beyond price, that may help stakeholders in low- and middle-income countries select quality-assured biosimilars.
The issue continues with a Perspective from Michael S Reilly and Ralph D McKibbin on misinformation about interchangeable biosimilars which they claim undermines US health policy, physician confidence, and patient health. The views of these authors have been aired before and readers will have to decide on whether they find them convincing.
This is followed by a short Special Report authored by Professor Irene Krämer and Dr Judith Thiesen on ‘Extended stability data on small molecule anticancer medicinal products – anything new? Any additional information necessary?’. The authors highlight that small molecules remain an essential part of combination chemotherapy, but note that although many studies on the extended stability of small molecule preparations have been published, not all licensed medicinal products and stability-determining factors are covered in these. Different dosages and concentrations, new types of containers, formulation changes of the starting material, and advanced administration technologies continuously require additional in-use stability studies.
The remainder of the issue comprises 21 short reports describing physicochemical stability determinations of numerous small molecule anticancer medicinal products, all by Professor Irene Krämer, Dr Frank Erdnuess and Dr Judith Thiesen. These investigate various reconstitution diluents and different containers. The products included in the study are Doxorubicin Accord, Epirubicin Accord, Idarubicin Accord, Mitoxantrone Accord, Bortezomib Accord, Irinotecan Accord, Topotecan Accord, Etoposide Accord, Vinorelbine Accord, Carboplatin Accord, Cisplatin Accord, Oxaliplatin Accord, Azacitidine Accord, Cytarabine Accord, Fluorouracil Accord, Gemcitabine Accord, Cabazitaxel Accord, Docetaxel Accord, Methotrexate Accord, Pemetrexed Accord and Fludarabine Accord. These reports identify appropriate storage times for the diluted products in defined containers and storage temperatures.
Robin Thorpe, PhD., FRCPath
Editor-in-Chief, GaBIJournal
Disclosure of Conflict of Interest Statement is available upon request.
Copyright © 2024 Pro Pharma Communications International
Permission granted to reproduce for personal and non-commercial use only. All other reproduction, copy or reprinting of all or part of any ‘Content’ found on this website is strictly prohibited without the prior consent of the publisher. Contact the publisher to obtain permission before redistributing.
Source URL: https://gabi-journal.net/what-to-look-forward-to-in-gabi-journal-2024-issue-2.html
It was with great pleasure that I assumed the role of Editor-in-Chief (EiC) of GaBI Journal in January of this year. Taking over the helm from Professor Philip D Walson is a considerable challenge; Phil’s excellent, thorough example will be very difficult to follow. My experience is restricted largely to biosimilars with which I have been involved since their concept and I will be relying on able colleagues for their expertise with generics! I hope to be able to carry out the important job of EiC effectively and efficiently.
In this issue of GaBI Journal, we have a number of papers on diverse topics.
In the first Original Research article Tomás Abbot, et al. describe budget impact analysis of Rixathon, a rituximab intravenous biosimilar in patients with follicular lymphoma and large B-cell non-Hodgkin lymphoma in a study conducted in Chile. They conclude that adoption of Rixathon biosimilar rather than the originator product resulted in clear overall cost savings. This clearly increases patient accessibility to rituximab treatment.
In the second Original Research article Dhananjay Panigrahi, et al. have conducted pharmacokinetic (PK) bioequivalence studies of a new Etoricoxib tablet formulation developed using proprietary MiST technology involving risk assessment and mitigation using commercially available software.
The simulated data generated were in line with the observed PK data obtained from the bioequivalence study. This work demonstrates application of predictive modelling and simulation tools to accelerate new product development.
Adjunct Professor Pekka Kurki has contributed a Perspective on Comparative efficacy studies of biosimilars: data versus theoretical risks, beliefs, and comfort. Professor Kurki is well known as a strong supporter of biosimilars and has been very active in development of regulatory processes for their assessment from their concept. His views on reducing the need for clinical efficacy studies have been the subject of numerous publications. His Perspective reviews the current status of regulatory guidance on clinical trials and encourages regulatory agencies, especially the US Food and Drug Administration, to take notice of the accumulating evidence for significant changes in the need for clinical efficacy studies.
Andriy Krendyukov, et al. present a Perspective on current understanding, knowledge, and perception of biosimilars in a changing landscape of regulatory requirements. They note that even in established biosimilar markets, understanding of biosimilar specific terms such as switching and extrapolation is variable and knowledge of evidence required for biosimilar development and approval is lacking and/or outdated. Lack of familiarity with these concepts and the evidence required to support biosimilar development may deter healthcare providers from using biosimilars to their full advantage.
More education for healthcare professionals is required in therapeutic areas where biosimilars are prescribed, and this should be updated regularly in step with evolving regulations.
To close, I wish everyone all the best for a happy and prosperous new year and encourage authors to submit relevant papers for consideration for publication in GaBI Journal.
Robin Thorpe, PhD., FRCPath
Editor-in-Chief, GaBIJournal
|
Editor’s note: |
Disclosure of Conflict of Interest Statement is available upon request.
Copyright © 2024 Pro Pharma Communications International
Permission granted to reproduce for personal and non-commercial use only. All other reproduction, copy or reprinting of all or part of any ‘Content’ found on this website is strictly prohibited without the prior consent of the publisher. Contact the publisher to obtain permission before redistributing.
Source URL: https://gabi-journal.net/first-2024-gabi-journal-issue-highlights.html
|
Abstract: |
Submitted: 8 December 2022; Revised: 8 December 2022; Accepted: 18 December 2022; Published online first: 8 December 2022
In the Opinion entitled Biosimilars drug development: time for a paradigm shift? in this issue of GaBI Journal, the authors question the need for what they consider to be the arduous regulatory requirements for approval of biosimilars [1]. The Opinion repeats already proposed and often published possibilities for changing and particularly abbreviating the established biosimilar approval process. These are the personal opinions of the authors and others will agree or disagree largely depending on their view of the current regulatory systems for assessing biosimilars and how these affect biosimilar development.
A significant factor which the authors claim supports their proposals is that, to date approved biosimilars have been shown to have noefficacy or safety concerns. This is certainly largely true for real biosimilars approved by experienced regulatory authorities (mainly in developed nations). But all of these have been approved using the current regulatory guidelines! Most of the approved biosimilars have been produced by ‘Big Pharma’ or subsidiaries of Big Pharma who have much experience with producing biological products andsignificant resources for this. Where this has not been the case, e.g. for copy products marketed in developing nations problems have arisen and quality, efficacy and safety of some of these products is suspect if not clearly compromised. It is therefore a possibility thatloosening the requirements for approval of biosimilars would result in unsatisfactory products.
Biosimilar approval requirements as detailed in the various guidelines produced by the relevant regulatory agencies are constantlyevolving, and are continuously updated to take account of experience gained and scientific, technical and clinical advances. The guidelines are thus living documents and not inflexible ‘tablets set in stone’. An example of this flexibility is the most recent draft of thebiosimilar guideline adopted by the Medicines and Healthcare products Regulatory Agency (MHRA) of the UK, which includes clearindications where clin ical efficacy trials are not needed. This type of trend is reflected in guidance from other regulatory jurisdictions. The general move towards more reliance on quality (chemistry, manufacturing, and controls, CMC) assessment (including the quality comparability assessment) and on clinical pharmacokinetics/pharmacodynamics (PK/PD) and less need for clinical efficacy andsometimes immunogenicity assessments is clearly ongoing, but the authors seem unaware of it. The authors’ opinion gives theincorrect impression that inflexible, unjustified regulations are hindering production of biosimilars; this does not seem to be the case at least in the developed world.
The desirability of ‘One global reference product’ is mentioned in the letter. There are two possible alternatives for this. Firstly, a ‘physical’ global reference product could be provided by some suitable organization, which could be used for biosimilar development by those who require it. Although this may seem rea- sonable (it has been proposed several times previously) there are serious problemswith it, such as who provides the product, who characterizes it, who dis- tributes it and how its stability and sustainability is guaranteed.Also, how does it relate to products used in the country in which the biosimilar is being developed and how are users and regulators to be convinced that it is an appropriate reference product for use in their jurisdiction?
A second approach would not provide the reference product as such, but nominate a commercially available reference product from one source which could be globally’ adopted by those who want to use this approach. This suffers from similar problems to the first approach mentioned above. In addition there are possible issues with continued availability of this as a reference product and ensuring consistent prod uct characteristics, as commercial products undergo development and change unpredictably over time. These are just some of the problems with this ‘global reference product’ concept.
The authors blame over arduous, unnecessary regulatory requirements for apparently poor uptake of biosimilars. However, evidence suggests that reluctance to use/ adopt biosimilars due to an unfounded suspicion of their quality, efficacy and safety by prescribers andpatients and often too little difference between the price of the biosimilar and the originator products are more likely reasons for this.
Biosimilars are now firmly established in most developed nations as copy biologicals with a clear and effective regulatory route for approval, which allows marketing of safe and efficacious biosimilar products. Although the regulatory requirements must (and do) evolve as experience and science progresses, this must be carefully evaluated to ensure that efficacy and safety are not compromised. If biosimilars are to increase in uptake as acceptable biological products it is important that they are perceived as being as accept- able as stand-aloneproducts by all involved in their production and use. Any perception that ill-advised, politically/financially driven pressures to inappropriately lower regulatory standards for their approval could seriously damage the acceptability of biosimilars.
Competing interests: None.
Provenance and peer review: Commissioned; internally peer reviewed.
Reference
1. Athalye SN, Mittra S. Biosimilars drug development: time for a paradigm shift? Generics and Biosimilars Initiative Journal (GaBI Journal). 2023;12(1):17-22. doi:10.5639/gabij.2023.1201.005
|
Author: Robin Thorpe, PhD, FRCPath, Deputy Editor-in-Chief, GaBI Journal |
Disclosure of Conflict of Interest Statement is available upon request.
Copyright © 2023 Pro Pharma Communications International
Permission granted to reproduce for personal and non-commercial use only. All other reproduction, copy or reprinting of all or part of any ‘Content’ found on this website is strictly prohibited without the prior consent of the publisher. Contact the publisher to obtain permission before redistributing.
Source URL: https://gabi-journal.net/response-to-the-opinion-entitled-biosimilars-drug-development-time-for-a-paradigm-shift.html
Author byline as per print journal: Professor John-Joseph Borg, PhD; Yolanda Elias Gramajo, MD; Professor Andrea Laslop, MD; Robin Thorpe, PhD, FRCPath; Jian Wang, MD, PhD
|
Introduction: Biosimilars have the potential to improve access to medicines for many across the globe. However, work is required to ensure adequate regulation, pharmacovigilance and education about biosimilars. Colombia implemented biosimilars regulation in 2017 and a 3rd Colombian Educational Workshop was organized by GaBI and the Instituto Nacional de Vigilancia de Medicamentos y Alimentos (INVIMA) in 2019 to follow up on progress and provide a forum for further discussion. |
Submitted: 9 April 2020; Revised: 8 June 2020; Accepted: 15 June 2020;; Published online first: 29 June 2020
Biosimilars or similar biotherapeutic products (SBPs), are a relatively new class of biotherapeutic agent. With appropriate regulatory and pharmacovigilance procedures in place, these products have the potential to improve access to medicines worldwide. These drug products are being developed and are entering markets across the globe. With sufficient trust in and uptake of these products, healthcare costs could be reduced dramatically.
Europe has been at the forefront of developing biosimilars regulation in recent years and now an internationally agreed system of regulatory approval is needed. Similarly, pharmacovigilance of biosimilars needs to be done on a global level. There are also questions regarding the interchangeability of biosimilars and a global understanding of this should be laid out. To achieve consensus on these points, open discussion across national borders and between different stakeholder groups is key.
To facilitate discussion concerning quality assessment of biologicals/biosimilars in Colombia, in 2016 and 2017, an educational workshop [1] and a follow-up meeting [2], were organised by the Generics and Biosimilars Initiative (GaBI) in collaboration with the National Food and Drug Surveillance Institute of Colombia (Instituto Nacional de Vigilancia de Medicamentos y Alimentos, INVIMA). Together, these meetings provided a forum to exchange knowledge on best practice and enabled the status of biosimilars quality assessment in Colombia to be viewed with clarity [3].
Following the implementation of biosimilar regulation in Colombia in 2017, a third meeting on the regulatory assessment of biosimilars in Colombia was held in 2019. This interactive workshop provided a forum for regulators, clinicians, pharmacists, academics and healthcare professionals from Colombia who are involved in biological/biosimilar medicines evaluation, to share knowledge and exchange information with expert speakers from Canada, Europe and the US. They engaged in active discussions that concerned the current status of biosimilars regulation in Colombia; standards and the stepwise approach of quality and immunogenicity assessment of biologicals/biosimilars; structure–function relationship of biological medicines; switching; pharmacological (pharmacokinetic (PK)/pharmacodynamic (PD)) and clinical studies of biosimilars; extrapolation of indications; post-marketing pharmacovigilance practices of biologicals/biosimilars to ensure patient safety; and future educational needs and how to improve the uptake of biosimilars.
Overall, the meeting aimed to bring experts together to clarify biosimilars regulatory concepts and concerns, in order to improve biosimilar regulation and increase their uptake in Colombia.
On 30 April 2019, GaBI held the 3rd Colombian Educational Workshop on Regulatory Assessment of Biosimilars. As with previous workshops [1–3], the aim was to review and explain the current status of biosimilars regulation in Colombia. The format was similar to that followed in prior scientific meetings and educational workshops as reported in GaBI Journal [4–6]. There were a number of expert speaker presentations followed by Q&A and an in-depth panel discussion. The presentations are downloadable from the GaBI website [7]. All participants were encouraged to engage in active discussion about the presentations given by expert speakers and to discuss selected case studies.
Presentations were in English or Spanish with simultaneous translations into Spanish or English, respectively.
The workshop began with a welcoming speech from Dr Lucia Ayala, Director of Medical Devices and Technologies at INVIMA. This included a brief introduction to the Colombian regulatory approach to biosimilars. The Austrian Medicines and Medical Devices Agency’s (AGES MEA) Head of Scientific Office, Professor Andrea Laslop, then provided a second welcome address. She celebrated the longstanding collaboration between INVIMA and GaBI and briefly outlined the workshop objectives (as summarized in the Introduction).
Biosimilars in Colombia: a year after regulation implementation
Mr Aurelio Enrique Mejía Mejía, Director of Medicines and Health Technologies at Colombia’s Ministerio de Salud y Protección Social, and Johanna Andrea García Cortes, Professional Specialist at INVIMA, gave presentations which discussed the implementation of Colombia’s Biotechnology Decree 1782/2014. Their presentations entitled ‘Colombia’s biological/biosimilar regulation: a year after its implementation’ and &lsqup;Biosimilar regulation in Colombia: one year later’, respectively, can be found on GaBI website [7].
In a brief summary, the two presentations outlined details of the 2014 Biotechnology Decree 1782. This laid out the requirements and procedures of INVIMA to evaluate the quality, safety and efficiency of biological medications and aimed to enable the appropriate approval and commercialization of such products in Colombia in the future. The two presentations discussed the decree and its impact following implementation in August 2017. In the first year of implementation, it has led to more therapeutic options being available to patients and an increase in competition in Colombia’s biological drug market. At present, 23 biosimilars are under review in Colombia, of which trastuzumab has undergone all regulatory processes and achieved marketing authorization. In addition, there are regulations in place to ensure that biosimilars enter the market meeting global standards of safety and efficacy. The next step is to improve the education of healthcare professionals to help increase the uptake of biosimilar products across the country.
Quality assessment of biologicals/biosimilars – most relevant quality attributes: case study on monoclonal antibody
Professor John-Joseph Borg, Malta Medicines Agency’s Director of Post-Licensing, discussed the quality assessment of biologicals/biosimilars in the European Union (EU) [8].
Professor Borg outlined the basic concept of a biosimilar:
He noted that, due to the complexity of biosimilars, it is not appropriate to follow the same approach as with simple generic drugs when addressing bringing biosimilars to market. As such, comparability exercises are required for biosimilars to be authorized in the EU.
In the EU, a complete and appropriate quality dossier is required for a biological product to be approved (Module 3). For a biosimilar, this must also include a comprehensive comparability exercise (quality, non-clinical, clinical), see figure 1. He added that establishing comparability is a stepwise approach and non-clinical and clinical data are required before product developers should move on to address the next step and address any residual uncertainty. Licensing decisions are then made based on the entire data package which includes quality, non-clinical and clinical parameters that demonstrate similarity to a reference product. All licensing is done on a case-by-case basis.
So, to build an application dossier for a biosimilar, a product developer will need a full Module 3, plus the comparability exercises (there should be multiple data points with all data being recorded over a period of time), followed by non-clinical studies and then clinical studies. If a product meets the requirements and is approved, conditions can then be attached to approval in the post-authorization phase.
Professor Borg further discussed the comparability evaluation and noted that all aspects mentioned above must be taken into account. This evaluation includes details of the nature and level of knowledge of the product, i.e. its complexity, structure-activity relationship, relationship between therapeutic and endogenous proteins and the mode of action. He also discussed aspects of immunogenicity and highlighted that this is an issue for all biological products. If a reference causes immunogenicity, so will a biosimilar. The risk factors for immunogenicity are both product and patient related.
Another key issue when considering biosimilars is that any variation in process can cause a different product to be produced, see figure 2. These variations can occur at any point during processing. Therefore, a regulator needs to know about every change made during production/processing and any effects that changes may, or may not, have. The sourcing and testing of the reference product must also be done over a period of time to account for any differences in the reference.
Overall for biologicals, the quality is highly dependent on the manufacturing process which is very complex. For a product to be accepted, it must meet quality criteria and be validated with safety and efficacy data. Professor Borg noted that there are additional critical quality aspects for a biosimilar and he went through a non-exhaustive list of these, see Table 1.
The EU Committee for Medicinal Products for Human Use (CHMP) guideline for comparability was discussed, see figure 3. This included notes on the origin of the reference product and how, when comparing a reference to a biosimilar, the same reference product (from the same country of origin) should be used over time.
Professor Borg gave an overview of the chemistry, manufacturing and controls (CMC) documents for monoclonal antibodies (mAbs) derived from a monoclonal cell line. This included a description of the development and production of mAbs and their characterization (physicochemical characterization; immunochemical properties; biological activity; information on purity, impurity and contaminants; and on quantity). The talk was finalized with an outline of Remsima biosimilar comparability where he included a comprehensive list of the studies comparing the physicochemical and biological activity of the Remsima biosimilar and the Remicade originator.
Pharmacological studies (PK/PD) to assess biosimilar medicinal products
Dr Jian Wang, Division Chief of the Clinical Evaluation Division, Biologics and Genetic Therapies Directorate, Health Canada, discussed biosimilar pharmacological (PK/PD) studies.
Biosimilars are similar to their brand-name reference products and not the same due to being made from different cell lines and by different manufacturing processes. To support regulatory approval, guidance/policy requests that comparisons between the biosimilar and its reference are made. These include, see Figure 4:
Clinical studies are needed to ensure that residual uncertainty from quality assessment does not cause clinically meaningful differences in efficacy, safety and/or immunogenicity in the sensitive population. Dr Wang stated that the main goal of clinical PK/PD studies is to rule out unacceptable PK/PD differences that could indicate the presence of significant structural and functional differences between a biosimilar and a reference product.
Regarding comparative PK studies, Dr Wang noted that these comparative clinical PK studies should be conducted in a setting that is reflective of the clinical situation and/or is sensitive to detect differences between the biosimilar and the reference. They should also be planned based on the characteristics of the reference, including its mode of action, safety profile and PK properties. In general, PK studies can be done on healthy volunteers. However, these individuals may not always reflect the PK parameters of patients. As such, comparative PK studies can also be conducted in the patient population.
The same principles of study design, statistical methods and criteria of acceptance for small molecules are used as a general guidance for biologicals. When the route of administration is intravenous (IV) which does not include an absorption phase, some additional parameters from elimination phase will be included for equivalence assessment.
In some aspects of study design, the single dose cross-over design is the most sensitive PK study design, for short half-life biologicals. However, this design can be limited by the properties of the biological such as having a long half-life or following the formation of antidrug antibody (ADA). In specific cases, parallel and/or multi-dose designs can be considered.
Many biologicals, including mAbs, cytokines, and growth factors, display target mediated drug disposition (TMDD), see figure 5. For such biologicals, three considerations must be made when conducting comparative PK/PD studies:
Critical quality attributes can influence the PK of a mAb and therefore, may have a direct impact on biosimilarity, see Table 2. In terms of immunogenicity, most biologicals induce some level of ADAs and these may have undesirable clinical effects on PK, efficacy and/or safety, including immunogenicity. It was also noted that PopPK studies are being used in demonstrating comparability for biosimilar mAbs as supportive studies.
Finally, on comparative PD studies, Dr Wang stated that PD studies are desirable, if feasible, and can help reduce residual uncertainty. PD parameters should be investigated as part of the phase III trial. He then discussed PD surrogates and aspects of PD sensitivity (including clinical, assay and dosing). Also, it is necessary to measure the baseline endogenous levels of a biological in blood plasma if the biological product is produced endogenously. In conclusion, for products with a reliable PD marker, a high quality and sensitive PD study (usually combined with PK) may be better than an efficacy study in terms of detecting differences in efficacy between a biosimilar and its reference product.
Head-to-head clinical studies and biosimilarity studies to assess biosimilar medicinal products
Dr Yolanda Elias Gramajo, Senior Clinical Evaluator, Clinical Trials Division, Health Canada, discussed head-to-head clinical studies and biosimilarity studies to assess biosimilar medicinal products.
Dr Elias Gramajo began by outlining that the pathway for biosimilar development and approval is designed to demonstrate similarity to its reference product with respect to quality, safety and efficacy. This uses a stepwise approach that is often depicted as a pyramid, see figure 6. This includes analytical, non-clinical and clinical studies. She gave a brief overview of the general regulatory requirements and the requirements for biosimilar development, see figure 7.
As part of the clinical programme for biosimilar development, comparability exercises are required. The comparative exercise objective is to demonstrate similarity in PK/PD, efficacy, safety and immunogenicity between the biosimilar and the reference product. In general, clinical trials are required (phase III for at least one indication) but in some cases PK/PD studies can suffice.
When it comes to the clinical development programme for biosimilar products, it is preferred that clinical trials follow an equivalence design. Here, a trial has the primary objective of showing that the response to two or more treatments differs by an amount which is clinically unimportant. This is usually demonstrated by showing that the true treatment difference is likely to lie between a lower and upper equivalence margin of clinically acceptable differences. She outlined some key considerations for comparative clinical trials including that generally 90%–95% confidence interval (CI) equivalence margin in the PP population (per-protocol) is acceptable, randomized design, double-blind/adequately powered, power and sample size sufficient to detect difference, dose and route consistent with reference.
Sensitive clinical study populations were then discussed, and that the comparative clinical study should be conducted in a sufficiently sensitive population that is representative of the authorized indications to detect differences between the biosimilar and its reference. The endpoint should be considered to improve the detection of potential differences between the biosimilar and the reference within the sensitive population.
When it comes to safety, immunogenicity is the most important aspect. Dr Elias Gramajo presented a number of points relevant to this including ADA formation. She also outlined the immunogenicity assessment strategy which includes screening assays, confirmatory assays, neutralizing assays and PK/clinical impact assessment. In all cases a biosimilar should never be more immunogenic than its reference in terms of ADA incidence or concentration.
In conclusion, when a biosimilar is authorized it can be granted all therapeutic indications held by the reference based on the totality of evidence obtained from all comparative analyses, see figure 8.
Extrapolation of biosimilars
Professor Andrea Laslop, Chair of the workshop, delivered a presentation on the principles of extrapolation of indications in the EU. Biosimilar extrapolation is when a biosimilar can be used for any indication that the reference product is approved for, even if the biosimilar itself has not been directly studied in a comparative clinical trial for that indication.
Professor Laslop outlined some general considerations for extrapolation, which is an important feature of the biosimilar approval process but that it continues to cause contention. Many EU biosimilar guidelines have been set up to address the issue and to date, extrapolation has been implemented in all biosimilar product approvals. She highlighted the fact that the concept is not new and has been used for biosimilars and generics and also in paediatric indications and other special populations. In addition, extrapolation can occur when there have been changes to the manufacturing processes of biologicals.
Concerning changes in the manufacturing process, comparability exercises are carried out to ensure the product efficacy and safety is not altered. When such changes are made, the product will be different and thus by definition, it will be a biosimilar (typically clinical data are not required to approve manufacturing changes).
Mechanism of action (active site) is key to extrapolation, see Table 3. This is mediated by functional molecular moieties in a disease-specific manner, which can be characterized by sensitive assays. If the same mechanism of action (MoA) or the same receptors are involved for the function of the biological/biosimilar product in different diseases, then extrapolation is straightforward. However, in some cases additional non-clinical or clinical data may be required, e.g. different active site, different receptor, different safety profile.
She noted that the overarching guideline on biosimilars states: if biosimilarity has been demonstrated in one indication, extrapolation to other indications of the reference product could be acceptable with appropriate scientific justification. Likewise, the general guideline on biosimilars containing biotechnology-derived proteins as the active substance, non-clinical and clinical issues, also says that extrapolation could be acceptable, but that in case of unclear relevance of the safety and efficacy data from one indication for another one, additional data will be required. In all cases extrapolation is only considered in light of the totality of evidence.
Professor Laslop presented a number of cases where extrapolation had occurred and justified the reasons for extrapolation in each example [9, 10].
In conclusion, extrapolation is essential for the success of biosimilars and must be done on the basis of the totality of data available. It is not done automatically and requires scientific justification. This is a common process in drug development and is not exclusive to biosimilars. Extrapolation is expected if comparability of the product, with respect to a reference, has been demonstrated on all levels. In addition, post-approval information for extrapolated indications is helpful and, to date, has shown the success of extrapolation.
Immunogenicity studies for assessing biosimilar products
Dr Robin Thorpe, Co-chair of the workshop, delivered a presentation on immunogenicity studies. This was similar to that given at the GaBI MENA 2018 meeting [6].
In conclusion, it was noted that immunogenicity issues occur all along the life cycle of a product and particularly when:
And that assessment requires:
Two further presentations were given by representatives from Amgen. ‘Biologicals and biosimilars – the complexity of structure and function’ was delivered by Dr Jennifer Liu, Director of Analytical Sciences, and ‘Considerations for product specific pharmacovigilance of multisource biologicals’ was delivered by Dr Thomas Felix, R & D Policy Director.
After the presentations, there was the opportunity for discussion about the topics covered. The key discussion points are summarized below.
The regulatory pathway in Colombia
The current status of biosimilars regulation in Colombia/The regulatory pathway in Colombia
Following the two presentations given on ‘Biosimilar’s regulation in Colombia: one year on’, there were some queries that required further clarification.
Dr Arley Gómez López expressed concern about the fact that Colombia does not have certain infrastructure in place for adequate drug analysis. Mr Mejía Mejía responded that the current regulation is in place to generate incentives and allow for the development of the infrastructure that is required. He emphasized that it is important to understand that the process is gradual. Having clarity regarding the standards, which has now been achieved, will allow companies to start to develop the capabilities in order to accomplish exactly the types of studies that are needed. Overall, Colombia’s Ministry of Health intends to give clarity regarding the norms so that they can be developed from the conditions. He also agreed that it is necessary to develop public and/or private initiatives to facilitate the development of the infrastructure.
Comparisons between the Colombian and other regulatory agencies
When asked about improved access to medicines in Colombia through commercial mechanisms, Mr Mejía Mejía stated that, at present, only hepatitis C medicines are bought through centralized purchasing. By focusing on the regulation of biotechnological medicines, it is hoped that access to medicines will be improved through the availability of greater therapeutic options which promote competition and reduce costs. Now that we have regulation in place, products are going through the approval process. When products are approved by INVIMA, they can start being prescribed by doctors and be covered by the health system. Eventually, in the case where the government and the ministry allow it, they can also be subject to centralized purchase or negotiations.
According to data in the presentations given, there seemed to be a lot of biosimilar applications in Colombia compared to the EU. Dr García Cortes advised that, when it comes to expensive medicinal products, it is good that there are a lot of biosimilar applications as this will promote competition and decrease prices. INVIMA’s Ms Alejandra Mayra Gomez Leal added that many biosimilars have been approved by the European Medicines Agency (EMA) and not the US Food and Drug Administration (FDA) and that Colombia is open to applications and whether or not they have been approved in other places may only be used as a reference.
There was a concluding comment by Andrea Carolina Reyes Roja, pharmaceutical chemist working at Misión Salud, a Colombian NGO. She stated that Misión Salud has followed the regulation process for biotechnological medicines in Colombia for more than 10 years. She congratulated the government for the emphasis it has put on the utilization of the abbreviated pathway as a public policy. Other health agencies, such as EMA, FDA and the World Health Organization (WHO), have a ‘questions and answers’ document published in October of 2018 which reaffirms the possibility of reducing clinical studies when supported by the vast knowledge of the molecules in analytical studies of high complexity and limited to PK/PD studies. The clarity that the Colombian government has provided on this issue will increase access and reduce the costs of medicines.
Following the presentation given by Professor Borg, Dr García Cortes wanted to know if Europe is thinking about removing the bridging studies. She noted that in Colombia they have found cases where there are significant differences between the product in the US and the European counterpart. In such cases, it is difficult to evaluate the comparability, so should bridging studies be removed? And in these circumstances should it be the US or EU product? And if only one reference product is taken, whether it be the European or the US. In response, Professor Borg noted that in the EU the reference product needs to be sourced in the EU to comply with comparability requirements. In addition, Andrea Carolina Reyes Roja stated that for the quality comparison, Europe requests the comparison to the European reference product and does not accept head-to-head comparison to a US-derived reference. She pointed out that this is different from the clinical development programme, where under certain conditions bridging exercises can be accepted. For example, a clinical study of the US reference could be used if it is also demonstrated that both the US and the EU reference product are sufficiently similar on the quality level.
Stepwise approach – PK/PD trials, comparability studies
When to use PK and PD studies and data
Ms Alejandra Mayra Gomez Leal was interested to know more about mAb studies and PK data collection. For the majority of mAb studies as presented by Dr Wang, the primary evaluation was for the efficacy aspects, and as a secondary objective, they evaluate the PK. Dr Wang explained that normally the first PK measurements will be done after the first dose of medication, and this essentially gives a single-dose PK. However, depending on how many samples can be collected, the study must be very well designed to collect multiple samples at different time points so that a PK profile can be created. In addition, and in general, PK data are collected at multiple dosing time points, so it is possible to have single-dose and multi-dose PK data.
Associate Professor Claudia Patricia Vaca González noted in her conclusion, that Dr Wang said that when there is a good indicator of PDs it can be more desirable to have a PK/PD study than a clinical efficacy study. She wondered how generalized this statement was, considering there is a growing interest from the agencies and countries to have competition and competitive products on the market. This approach could improve the speed of introduction of these products into the market. Dr Wang responded by noting that this statement is not possible to generalize to all biologicals. He reiterated that for products with well-known, well-established PD surrogates, you can generally use comparative PK/PD studies. However, agencies may also ask for a longer-term safety study which may not be powered to demonstrate equivalence and the results of which cannot be inferred from the comparative PK/PD study.
The science and rational of clinical trials
Rejection after clinical trials
There was a query regarding the number of biosimilars that were rejected in Canada, following clinical trials. Dr Wang stated that, when it comes to biosimilars and clinical trials, it is not purely a science issue, but also a regulatory issue. A biosimilar should be as good, or as bad, as the reference. If it is better, it becomes a judgement call. How much better is it? And is that going to cause safety concerns or not? In biologicals, it is often the case that you will have better efficacy but a worse safety profile. So, a proper benefit-risk assessment must be made and within the considerations of the country’s regulations. Overall, the situation is quite complicated, it is not the case that products go through all steps prior to clinical trials, without hitch, and then get rejected on the basis of trial results.
The importance/discussion of pharmacovigilance, naming issue
Improving and maintaining pharmaco-vigilance
Associate Professor Claudia Patricia Vaca González made some comments on the naming of biologicals. She said that WHO allowed countries the freedom to establish differentiation from the common international names of products. This came after lengthy discussions about both the inconvenience of having differentiation in nomenclature which causes confusion between patients and doctors; and following concerns expressed by different countries that this name differentiation could be used to reduce competition when generic or biosimilar medicines enter the market. In addition, she noted that nomenclature is very important when it comes to pharmacovigilance and tracing of the active principle. It is important to have information related to the product batch and the ability to trace a product through its logistic chain. She stated that health systems in all countries must improve upon traceability to improve pharmacovigilance.
Dr Felix responded that the concept of active ingredient traceability is very important. This is how small molecules are traced around the world. However, active ingredient traceability and batch level traceability are not two things that necessarily go together. In most countries, it is not possible to find the manufacturer of a product with only the non-proprietary name product batch number.
Professor Laslop agreed that it is important to have separate pharmacovigilance reporting for each individual biosimilar product. In Europe, pharmacovigilance data on the non-proprietary name would not be collected alone. The European implementation pathway instead requires prescription according to brand name. That is, in Europe, biosimilars are never prescribed according to non-proprietary name but rather by specific brand name together with the batch number, and this is how a product can be traced.
Dr Felix added that Europe has not implemented a specific naming approach and some countries outside Europe see this as a greenlight to do the same. However, they do not take into account certain aspects of European legislation in place to improve traceability which include brand level prescribing, good pharmacovigilance guidance and education of healthcare professionals.
With respect to this discussion, Professor Borg noted that new regulation is coming into force in the EU with respect to the falsified medicines directive. All batch numbers will be recorded where dispensed. Ideally in the future, all will be linked centrally at EMA with the help of IT software. Dr Felix explained that the directive is a European legislation which is in place to prevent the ability of counterfeit medications entering into the European system. As such, there is very high accuracy in the traceability of biological products and all products that enter Europe. In the future, this has potential to be a powerful tool and to improve patients’ safety, particularly if data input into the system occurs at the dispensing level.
A final comment was made by a member of the audience regarding pharmacovigilance and residual uncertainties. He expressed concern that these medicines were being released to the market despite the existence of uncertainties. In response, Dr Felix stated that, for all medicines, regulatory approval pathways are built on the best available evidence at a given point in time. Even for an innovative product, there is still some residual uncertainty that might exist, and the study of products must continue after they are approved. This is the case, particularly when they are used in patient populations that were excluded in clinical trials or inpatient populations that were not studied originally. In all circumstances, the collection of aggregate information is required to show that the benefit continues to outweigh risks. This is going to be especially important in the next wave of innovative medications that are being developed for patients with rare diseases which are based on clinical trial data sets that are much smaller. These will be promising in terms of their clinical benefit but due to their nature, there will be all the more reason for post-approval traceability of these products and continued measurement of the benefit-risks related to them.
Immunogenicity
After Dr Thorpe’s presentation on immunogenicity, Professor José Orozco asked if it is possible for a biosimilar to be less immunogenic. Dr Thorpe explained that there are instances where immunogenicity, at least appears, to be lower for a biosimilar. Often this is due to assay artefact problems and the real problem is that when assays are carried out the antigen must be selected with extreme care. The most logical way of doing this is to measure the antibodies against the product that the patients have received. The patients who have received a biosimilar, the new biosimilar, get screened against the biosimilar and the ones who have received the innovator get screened against that. However, this is labour intensive. As such, it is common to use just one antigen – and all the patients get screened against one antigen. This is allowed in the EU if the antigen is the biosimilar itself, as here you increase the possibility of detecting antibodies against a biosimilar which gives you a possible, slightly higher apparent immunogenicity of the biosimilar. In other circumstances, immunogenicity can be reduced in a biosimilar. This can be due to assay effects or may be because of high purity of the biosimilar (compared to older reference product made with less advanced technology). When a biosimilar has less immunogenicity, this seems good, however, this should ideally be justified in the assessment in terms of purity or assay issues.
There was a panel discussion chaired by Professor Laslop and co-chaired by Dr Gramajo.
The Regulatory panel discussion was introduced by Professor Laslop. The panel included Arley Gómez López, Research Director from the University Research Foundation ‘de la Salud’; Juan Fernando Juez Castillo, INVIMA; and Judy Hasleidy Martínez Martínez, INVIMA. Professor Laslop opened discussions and noted that the workshop presentations had thus far brought to light the two main pillars for assessment of biosimilars: the quality comparison (which includes non-clinical data) and the comprehensive clinical comparison.
Reducing the biosimilar assessment process
Mr Castillo noted that it is evident that we still have a lot to learn when it comes to biosimilars and their assessment. There is a great deal of complexity when it comes to biosimilars and their production. Therefore, it is very important to have a very strict process for analyses in Colombia. For now, he believes that shortening any analysis could result in a fall into reductionism, which is to be avoided. However, it may be necessary to have public and/or private concessions as neither the universities nor the government alone currently have the capacity to realize these types of complex analyses adequately.
When it comes to reducing the comparability exercise and the clinical studies for biosimilars, Mr Castillo also noted that this should only be done on a case-by-case basis. It is not possible to generalize and say that a certain category of products should follow a certain abbreviated ‘third pathway’ with less information required.
To emphasize this he noted that some mAb patents are expiring and, despite extensive characterization, there are still many uncertainties about the molecules. However, this is not the case for molecules like insulins which are well understood.
Dr Martínez Martínez noted that in Colombia the concept of a third pathway for certain drug products with reduced trials has been discussed. She explained that, Colombia’s Decree 1782 aims to ensure molecules are precisely characterized, have robust pharmacovigilance and good safety information. These molecules undergo clinical trials until enough information is known to prove their safety (either in Colombia or in other countries). In some cases, smaller biological molecules, such as insulins, heparins and filgrastim, can be well characterized and do not require as many clinical trials. Such molecules could be considered in the third pathway. However, to date, not many products have followed this third pathway. Overall, INVIMA is working with comparability to try and reduce the clinical and preclinical trials needed for some products but this should never impact on product safety. At present, INVIMA has not worked on the specific criteria for the different pathways. Laboratories can present the information through the pathway they chose based on the information and justifications that they selected throughout the trial. In general, if a characterization does not seem sufficient to the regulator, then more information is requested.
Professor Laslop added that this third pathway approach is similar to those adopted in Europe, Canada and the US. Here, there is potential to waive full clinical trials for certain less complex biosimilar molecules. However, if Colombia wants to adopt a similar approach to those nations, the guidelines and definitions need to be very clear. This is particularly important in terms of molecule complexity and what is, and is not, to be included in each of the different approval pathways.
In addition, Ms García Cortes noted that she did not support the idea of having a list of molecules in a third pathway. Biologicals should be assessed on a case-by-case basis, running through the three steps. These steps investigate the complexity of the molecule, the complexity of its MoA and the complexity of its production. Changes in production method such as a change in vial, can lead to massive adverse effects in the product that are not due to the molecule itself. As such, creating a list of molecules to be included in a third pathway does not seem plausible as their effectiveness is also dependent of the complexity of their action mechanism and production method.
A member of the audience noted that a third pathway should exist to give clarity in cases where it is not necessary to get to the end of the clinical trials and safety and efficacy studies. In such cases, PK/PD studies are carried out and the medicines are widely known and have robust pharmacovigilance. However, it is imperative not to compromise safety and INVIMA performs exhaustive evaluations to ensure this.
Another audience member also noted that research ethics should be part of the regulation because it ensures that patients’ rights are observed.
The applicability of the assessment pyramid
When a biosimilar undergoes evaluation for assessment of comparability, it should generally follow the stepwise approach outlined in the assessment pyramid. However, in many cases, not all stages of the pyramid are reached and undertaken prior to product approval. As such, it was proposed that this pyramid should be changed. Professor Laslop stated that she would not be in favour of removing or altering the pyramid as it is still the default pathway for biosimilar development, biosimilar assessment and, ultimately, biosimilar approval. In Europe, the possibility for abridged clinical assessments is exactly defined in product specific guidelines.
Dr Gramajo noted that the situation is the same in Canada. All assessments are done on a case-by-case basis. Those developing biosimilars should consult with agencies at an early stage to determine what information is needed and which trials are necessary. As such, the overall pyramid is still relevant.
Clinical trials
Dr Thorpe stated that classically, to prove clinical efficacy, a classical efficacy trial should be carried out. This is the standard and remains valid. However, there can be occasions when there is a better way of establishing clinical efficacy than performing a classical clinical trial. For example, with G-CSF (filgrastim) it is possible to determine PD and PK measurements more accurately than you can measure clinical responses. Clinical efficacy trials can still be carried out, but to the best of his knowledge, when these were carried out in Europe with filgrastim, the outcome was the same as shown by PK/PD studies. However, this does not mean that clinical trials do not need to be carried out with other products. The omission of clinical trials always needs to be justified.
According to Mr Castillo, if one arrives at the PK/PD step and there is little uncertainty, then this is when there seems little sense in continuing to clinical trials. They are unlikely to provide additional information. However, if there are many uncertainties following PK/PD studies it is unethical to continue to clinical trials. He believes that too many clinical trials are requested in the EU and North America. Many of these trials are huge, requiring many patients over a prolonged period of time and sample sizes required could exceed those needed for innovator products. Mr Castillo again affirmed that such decisions should be made on a case-by-case basis. He also highlighted that in Colombia, clinics are struggling to find enough patients with which to carry out large clinical trials. This is due to how the healthcare system is constructed. However, he hopes that this is changing so that more continuous studies can be done to assess long-term efficacy and trace adverse effects.
WHO reliance assessment
Mr Castillo noted that biosimilarity has not yet been officially defined in Colombia. This is an issue when choosing the exact pathway to follow for similarity assessment. It can also lead to redundant studies being done that have already been carried out in other countries.
In response, Professor Borg highlighted that WHO has a reliance assessment that helps regulators outside the EU assess biological products. As part of this, WHO has a formal agreement with EMA that allows EMA’s CHMP assessment report to be shared so that product assessment can be targeted on areas which are relevant to the country. As such, they do not need to waste time or money on reassessment and revaluation. This aims to allow for faster access to medicines for patients and improved healthcare systems in the non-EU countries. He suggested that Colombia could take advantage of this WHO reliance assessment.
Biosimilar education of the medical and patient community/Improving education about biosimilars
Professor García Cortes noted that the implementation of Decree 1782 is a big challenge for Colombia. Medical doctor education is a key part of ensuring its success. Colombia has done a lot of work to ensure correct evaluation of biosimilars from a qualitative, safety and efficacy point of view. It is now important that doctors have clarity about and trust in the medicines approved. As such, INVIMA’s next goal is to ensure that doctors and healthcare personnel are well educated when it comes to biosimilars. They should understand what they are and should trust the information available. She believes that, through this, INVIMA can create confident prescribers and good therapeutic results.
Mr Castillo stressed the importance of having a medical community that has knowledge and trust in the medicinal products it prescribes. INVIMA is working hard to ensure products receive a comprehensive evaluation and that there are channels of communication open to prevent any issues from causing problems or harm. With these mechanisms, and any other means, INVIMA will reduce the impact on the public health of Colombians.
Professor Laslop concluded that education of the medical community and the patient community is extremely important. In Europe, it became quickly apparent that it is not always efficient to simply publish something on a website. Instead, proactively approaching all stakeholders (the pharmaceutical manufacturers, or the patients, or the medical community) to educate, explain and communicate, has had far greater impact.
Dr Néstor Álvarez Lara noted that, when it comes to the communication of information, it is important to pay close attention to pharmaceutical marketing in Colombia. Advertising must be kept in check to ensure it does not negatively affect government spending or patient access to medicines.
Regulatory panel discussion conclusion and future actions
Dr Gramajo stated that the subjects discussed are very controversial, and there are a lot of things to consider which require more communication, more information, more collaboration between different agencies. Colombia is unique in that it is going to determine its own regulations and elect medical authorities in accordance to public opinion at a national and an economic level.
Discussion groups were provided with data on two semi-fictional trastuzumab biosimilar candidates. They were provided with physicochemical characteristics, selected glycan and biological attributes, and the results of a phase I study for Candidates 1 and 2.
Following the same format as previous GaBI meetings, each discussion group was asked whether the data for the candidates qualified for biosimilarity with a reference product from a quality (CMC) perspective. If not, they were asked what steps they would recommend fixing this. Discussion groups were also asked how ‘residual uncertainty’ could be addressed in preclinical or clinical studies. They were then asked, given that Candidates 1 and 2 had both the CDR (complementarity-determining region) and Fc (fragment crystallizable) region involved in their MoA for some of the indications, whether they would recommend extrapolation to all indications.
There were six discussion groups that evaluated the case studies. Overall, they all concluded that Candidate 1 is a biosimilar, from a quality perspective. However, there are differences between the candidate and the reference and some elements of residual uncertainty which require further investigation. If results of these investigations are as expected, then extrapolation is acceptable. When considering Candidate 2, all groups concluded that this is not a biosimilar, from a quality perspective. The differences between it and the reference cannot be solved and residual uncertainty is too large to warrant further study or clinical trial. Extrapolation is not acceptable.
Group 1 was moderated by Professor Fabio Ancizar Aristizábal Gutiérrez, and co-moderated by Judy Hasleidy Martínez Martínez. Based on the data presented for Candidate 1 this group suggested that further physicochemical or in vitro tests should be carried out to remediate differences. In addition, potency studies should be carried out. To address residual uncertainty, preclinical models could be used in vitro or in a parallel animal model. Here, clinical evaluation may be required for PK/PD data. Group 1 stated that Candidate 1 did qualify for extrapolation if the results obtained from the required physicochemical studies and in vitro studies resolve the uncertainties related to the quality attributes mentioned (fucosylation – antibody-dependent cellular cytotoxicity (ADCC); glycosylation – complement-dependent cytotoxicity (CDC) given that the therapeutic indication studied was relevant. Regarding Candidate 2, there are differences in some quality attributes, a larger sample of batches must be available to reduce uncertainty. Clinical studies do not allow the differences to be resolved, so do not recommend as biosimilar.
Professor Gutiérrez noted that having open communication channels and strong teamwork are very important when assessing biosimilars. This ensures everyone analyses and understands critical variables rather than criticizes information. Analysis methodology is important to optimise time use and to reduce questions following analysis. These case studies showed that the manner in which information is exchanged between different levels of experience in technical areas is critical. In addition, another important aspect is quality. The case studies put forward two quality parameters in the form of clinical trials. If preliminary quality results are obtained that raise doubt about the efficacy in the clinical trial, these can be used to confirm biosimilarity of a candidate product. In addition, Group 1 felt that the extrapolation of uses should only be allowed with better information regarding MoAs for each indication to know if they are complimentary. This is what was shown in the clinical trial provided.
Group 2 was moderated by Associate Professor Claudia Patricia Vaca González and co-moderated by Joseph Sebastián Cepeda Santamaría. The group confirmed similar outcomes to Group 1. They discussed that it is very important to compare the primary structures, yet in these cases there was no data with respect to that. It was also noted that there was no comparability data or immunogenicity data. For Candidate 2, they observed that some parameters recorded were outside the ranges expected to directly impact the immunogenicity and as such, the exercise did not enable the evaluation of immunogenicity.
Group 3 was moderated by Arley Gómez López and co-moderated by Gloria Cecilia Peñuela Sánchez. During their discussions, Group 3 noted that for Candidate 1, from a quality perspective, there are differences in the acid charge profile and the profile of deamidation which would affect the potency of the product. To remedy the differences, they should be evaluated in terms of their impact on the potency with clinical studies. They suggested that the residual uncertainty should be evaluated with the use of a small clinical study which is sufficiently sensitive in early stages of the disease. If this can be carried out, then extrapolation is possible. However, the group also noted that extrapolation cannot be done because the bioequivalence study was carried out on a single dose in healthy subjects and a more complete PK study would be required. When evaluating Candidate 2, Group 3 noted that it does not meet criteria to be a biosimilar from a quality perspective. The differences cannot be solved, and a clinical study and extrapolation should not be carried out.
Group 4 was moderated by Dr Néstor álvarez Lara and co-moderated by Giovanny de Jesús Otálvaro Rojas. This group’s opinion of Candidate 1 was aligned with that of Groups 1–3. In discussion about Candidate 2, it was noted that the clinical study design was not of good quality and the efficacy of the candidate was low.
Group 5 was moderated by Mr Castillo and co-moderated by Deyanira Duque Ortíz. With regards to Candidate 1, Group 5 noted that they had some concerns about the differences in the acid charge profile and ADCC binding test which could directly impact the PK and lead to inferior results. They suggested that information is needed to support the differences in acid charge profile. With regards to residual uncertainty, they noted that they would need the secondary evaluation results of overall survival (OS) and progression-free survival (PFS). In addition, they wanted clarification as to why the PCR evaluation variable was the primary evaluation variable. Overall, Group 5 said the candidate could be extrapolated but they would want to address the specific implications for gastric cancer.
Other observations the group made included:
Mr Castillo highlighted some brief adjustments in examinations that influenced the part of the bond strength, the power. The differences in glycosylation also affected these factors. In the PK table, with reference to the higher value, which is the expected value, the comparator result was lower than the expected value but not by much whilst the reference value was within or even higher. From an efficacy level, it caught the attention that even with these differences, the biosimilar presented a slightly higher efficacy compared to the reference, about 0.2% higher than the reference.
Group 6 was moderated by Johanna Andrea Garcia Cortes, and co-moderated by Ivan David Fonseca García. With regards to Candidate 1, the group noted that charge profile and deamidation were observed in the fucosylation particles. It was explained that the former affects ADCC and the latter, potency. However, when reviewing the data of ADCC, CDC and binding tests, they all fall within the required parameters. In addition, the group found it striking that there was nothing about comparison of comparative primary structure or comparative immunogenicity. For Candidate 2, the PK data endpoints do not fall in the correct regions and thus it is not a biosimilar.
In addition to the points made by the group moderators, Dr Wang noted that interestingly in the case of Candidate 1, the PK data is very similar to the reference. If this case had a true PD surrogate you might be able to determine a difference, but here you have no PD data so clinical studies are needed. However, looking at this case, you will need a sensitive study population as the PK values for the two products are comparable; if you had a non-sensitive study population you may reach a wrong conclusion. At each step, comparison must be sensitive to detect potential differences.
Ms Sánchez noted that the case studies were useful as it allowed workshop participants to have a complete discussion about both quality evaluation and clinical studies and the different parameters that can affect quality. Quality is very important when it comes to a products efficacy and safety and it allows for faster conclusion about whether a product is a biosimilar.
Professor Borg concluded that there was an issue with the clinical studies. The studies for the two candidates have two different designs and this could have been further discussed during the workshop. In addition, the primary endpoints warranted further discussion. For one candidate this was the overall response rate (ORR), which he believes is not the best endpoint for a study. He noted that the results clearly show that, even with an insensitive endpoint, there are huge differences in the efficacy of the product. This clearly demonstrates an inferior product. With this in mind, he added that the take home message is to consider the totality of evidence when in decision-making.
The 3rd Colombian educational workshop was successful in bringing together those involved with biological/biosimilar regulation in Colombia with experts from Canada, Europe and the US. It highlighted the progress that has been made in Colombia in terms of biosimilars regulation since the 2018 implementation of Decree 1794 and the future steps that are needed to improve biosimilars uptake and access to medicines. The workshop also highlighted many important issues surrounding biosimilars regulation and regulatory assessment and helped to clarify many regulatory concepts and concerns. The attendees shared ideas with the speakers and received clarification on issues of interest and concern.
The Generics and Biosimilars Initiative (GaBI) wishes to thank Professor Andrea Laslop and Dr Robin Thorpe, Chair and Co-chair of this workshop; the moderators and co-moderators in implementing the parallel discussions and clarifying information of the parallel discussion when finalizing the meeting report; as well as Mr Francisco Javier Sierra Esteban of INVIMA for his strong support through the offering of advice and information during the preparation of the workshop.The authors would like to acknowledge the help of the workshop speaker faculty and all participants, each of whom contributed to the success of the workshop and the content of this report, as well as the support of the moderators and co-moderators in facilitating meaningful discussion during the parallel discussions and case study working sessions, presenting the discussion findings at the meeting, and contributing in the finalization of this meeting report.
Lastly, the authors wish to thank Ms Alice Rolandini Jensen, GaBI Journal Editor, in preparing and finalizing this meeting report manuscript and providing English editing support on the group summaries.
Speakers
Professor John-Joseph Borg, PhD, Malta
Yolanda Elias Gramajo, MD, Canada
Thomas Felix, MD, USA
Johanna Andrea García Cortes, MSc, Colombia
Professor Andrea Laslop, MD, Austria
Jennifer Liu, PhD, USA
Aurelio Enrique Mejía Mejía, MSc, Colombia
Robin Thorpe, PhD, FRCPath, UK
Jian Wang, MD, PhD, Canada
Moderators
Néstor Álvarez Lara, PharmD
Professor Fabio Ancizar Aristizábal Gutiérrez, PhD
Joseph Sebastián Cepeda Santamaría
Deyanira Duque Ortíz, MSc
Ivan David Fonseca García
Johanna Andrea Garcia Cortes, MSc
Arley Gómez López, MD, PhD
Juan Fernando Juez Castillo
Judy Hasleidy Martínez Martínez
Giovanny de Jesús Otálvaro Rojas, PharmD
Gloria Cecilia Peñuela Sánchez, PharmD
Associate Professor Claudia Patricia Vaca González, MSc
Speakers and moderators had provided feedback on the regulatory panel discussion and the case study group discussion, respectively; read and commented the revised content of the manuscript, and approved the final report for publication.
Competing interests: The workshop was sponsored by an unrestricted educational grant to GaBI from Amgen Inc.
Provenance and peer review: Not commissioned; externally peer reviewed.
Professor John-Joseph Borg, PhD, Malta
Yolanda Elias Gramajo, MD, Canada
Professor Andrea Laslop, MD, Austria
Robin Thorpe, PhD, FRCPath, UK
Jian Wang, MD, PhD, Canada
References
1. Generics and Biosimilars Initiative. First INVIMA Educational Workshop on Assessment of Similar Biotherapeutic Products 2016; 14 June 2016; Bogotá, Colombia. Available from: www.gabi-journal.net/about-gabi/educational-workshops/first-invima-educational-workshop-on-assessment-of-similar-biotherapeutic-products-2016
2. Generics and Biosimilars Initiative. Second Colombian Scientific Meeting on Quality Assessment of Biosimilars/Similar Biotherapeutic Products 2017; 15 August 2017; Bogotá, Colombia. Available from: www.gabi-journal.net/second-colombian-scientific-meeting-on-quality-assessment-of-biosimilarssimilar-biotherapeutic-products-2017
3. Gray E, Matejtschuk P, Thorpe R. Quality assessment of biosimilars in Colombia – reducing knowledge gaps. Generics and Biosimilars Initiative Journal (GaBI Journal). 2018;7(2):79-83. doi:10.5639/gabij.2018.0702.017
4. Generics and Biosimilars Initiative. First Latin American educational workshop on similar biotherapeutic products, Mexico; 20 January 2015; Mexico City, Mexico. Available from: www.gabi-journal.net/first-latin-american-educational-workshop-on-similar-biotherapeutic-products-mexico-city-mexico-20-january-2015.html
5. Walson PD, Thorpe R. First MENA educational workshop on regulation and approval of similar biotherapeutic products/biosimilars, Dubai, United Arab Emirates, 1 September 2015. Generics and Biosimilars Initiative Journal (GaBI Journal). 2015;4(4):173–7. doi:10.5639/gabij.2015.0404.039
6. Laslop A, Wang J, Thorpe R. 2nd MENA Stakeholder Meeting on Biosimilars 2018 – Report. Generics and Biosimilars Initiative Journal (GaBI Journal). 2019;8(2):76-87. doi:10.5639/gabij.2019.0802.009
7. 3rd Colombian educational workshop on regulatory assessment of biosimilars 2019. 30 April 2019, Bogotá, Colombia. Available from: www.gabi-journal.net/about-gabi/educational-workshops/3rd-colombian-educational-workshop-on-regulatory-assessment-of-biosimilars-2019
8. European Medicines Agency. Guideline on similar biological medicinal products containing biotechnology-derived proteins as active substance: quality issues (revision 1). 22 May 2014 [homepage on the Internet]. [cited 2020 Jun 29]. Available from: https://www.ema.europa.eu/en/documents/scientific-guideline/guideline-similar-biological-medicinal-products-containing-biotechnology-derived-proteins-active_en-0.pdf
9. European Medicines Agency. Guideline on similar biological medicinal products. 23 October 2014 [homepage on the Internet]. [cited 2020 Jun 29]. Available from: https://www.ema.europa.eu/en/documents/scientific-guideline/guideline-similar-biological-medicinal-products-rev1_en.pdf
10. European Medicines Agency. Guideline on similar biological medicinal products containing biotechnology-derived proteins as active substance: non-clinical and clinical issues. 18 December 2014 [homepage on the Internet]. [cited 2020 Jun 29]. Available from: https://www.ema.europa.eu/en/documents/scientific-guideline/guideline-similar-biological-medicinal-products-containing-biotechnology-derived-proteins-active_en-2.pdf
|
Author for correspondence: Robin Thorpe, PhD, FRCPath, Deputy Editor-in-Chief, GaBI Journal |
Disclosure of Conflict of Interest Statement is available upon request.
Copyright © 2020 Pro Pharma Communications International
Permission granted to reproduce for personal and non-commercial use only. All other reproduction, copy or reprinting of all or part of any ‘Content’ found on this website is strictly prohibited without the prior consent of the publisher. Contact the publisher to obtain permission before redistributing.
Source URL: https://gabi-journal.net/3rd-colombian-educational-workshop-on-regulatory-assessment-of-biosimilars-2019-report.html
Author byline as per print journal: Robin Thorpe, PhD, FRCPath; Elwyn Griffiths, PhD, DSc; Niklas Ekman, PhD
|
Abstract: |
Submitted: 19 April 2018; Revised: 12 July 2018; Accepted: 18 July 2018; Published online first: 25 July 2018
Similar Biotherapeutic Products (SBPs or biosimilars) are being increasingly developed worldwide. The presence of this new class of biotherapeutic agent is improving access and availability to treatment for patients across the globe. However, the regulation and approval of biosimilars is not straightforward and practices differ from country to country. To ensure that biosimilars successfully enter markets and maintain the safety and efficacy achieved by their originator products, methods for their approval and regulation need to be laid out clearly.
To discuss the regulation and approval of biosimilars across the nations of Southeast Asia, the First ASEAN Educational Workshop on Regulation and Approval of Biosimilars/Similar Biotherapeutic Products took place on 23 July 2017, Bangkok, Thailand [1]. This was organized by the Generics and Biosimilars Initiative (GaBI) in collaboration with the Association of Southeast Asian Nations (ASEAN). Forty-three participants, including the speakers, attended the workshop.
This First ASEAN Educational Workshop on Regulation and Approval of Biosimilars/Similar Biotherapeutic Products was an interactive workshop that focused on the regulation and approval of biosimilars. It brought together regulators and key representatives from the ASEAN ACCSQ–PPWG (ASEAN Consultative Committee for Standards and Quality Pharmaceutical Product Working Group) Member States: Indonesia, Lao PDR, Malaysia, Myanmar, Philippines, Singapore, Thailand, Vietnam; along with academics, medical practitioners/specialists, pharmacists, and procurement specialists. These participants held discussions and exchanged information with experts from across Asia, Europe and the US.
One of the key aims of the educational workshop was to address the potential differences in quality as well as the therapeutic and immunological (immunogenicity) effects of biologicals across ASEAN nations. To facilitate this, representatives from regulatory authorities, academia and medical specialists, that are involved in biological and biosimilar development and approval in ASEAN Member States, were joined by expert speakers from other nations. The participants engaged in active discussions covering topics concerning: the principles and challenges related to manufacturing process development of biosimilars; the clinician’s experience of biocopy* erythropoietin (EPO); the regulatory experience of re-evaluating EPO; and the identification of future educational requirements.
The format of the First ASEAN Biosimilars Educational Workshop was similar to that followed in prior educational workshops as reported in GaBI Journal [2–4]. For more details of methods and case presentations, see the published report of the First Latin American educational workshop on similar biotherapeutic products [2], the First MENA educational workshop on regulation and approval of similar biotherapeutic products/biosimilars [3], and the First Turkish interactive workshop on regulation and approval of similar biotherapeutic products/biosimilars [4].
The ASEAN workshop began with presentations given by expert speakers [1]. The details of most of these presentations were updates to those given at other GaBI workshops and are summarized in their published reports [2–5].
Dr Thijs J Giezen, a hospital pharmacist at the Foundation Pharmacy for Hospitals in Haarlem, The Netherlands, and a member of the Biosimilar Medicinal Products Working Party (BMWP) of the European Medicines Agency, discussed the safety assessment and risk management of biosimilars, as reported in [2, 5]. However, in this more recent 2017 presentation, he highlighted that in many nations across the globe, patients and physicians have a knowledge gap when it comes to biosimilars. He advised that globally, further steps need to be taken to improve education and to increase trust in biosimilars.
Biocopy* EPO’s in Thailand
In addition to the presentations that have been given at previous GaBI workshops, two ASEAN-specific presentations were given. Professor Kearkiat Praditpornsilpa of Chulalongkorn University, Bangkok, Thailand gave a presentation entitled, ‘Clinician’s experience of biocopy EPO in Thailand’. Here, he discussed the well-documented immunogenicity of recombinant human erythropoietin (r-HuEPO) by subcutaneous exposure. This adverse immunological effect causes anti-r-HuEPO-associated pure red cell aplasia (PRCA). Professor Praditpornsilpa highlighted the fact that there have been increasing cases of anti-r-HuEPO-associated PRCA by subcutaneous exposure in Thailand. It is suggested that the immunogenicity may relate to human leukocyte antigen (HLA) immunogenetics, protein aggregation, stability during storage; and handling of drug products, formulation and drug product quality. Professor Praditpornsilpa and his research group have carried out extensive investigations into the unreliability of biocopy EPO’s in Thailand.
r-HuEPO’s have been licensed for the treatment of renal anaemia in Thailand and include innovator products and more than 20 biocopy products. However, there are inconsistencies in product characterization and quality which may lead to different immunogenicity and safety profiles. As such, the Prospective Immunogenicity Surveillance Registry of r-HuEPO with subcutaneous exposure in Thailand estimated the incidence rate of anti-r-HuEPO associated PRCA among subjects who had subcutaneous exposure to any currently marketed r-HuEPO product. In addition, the registry addressed the risk of anti-r-HuEPO associated PRCA and the association of product quality with adverse immunogenicity.
Following their investigation, the registry suggested that there is an association between product quality and immunogenicity. All anti-r-HuEPO associated PRCA cases had received biocopy r-HuEPO products, resulting in the observation of a correlation between product characteristics and adverse immunogenicity. As patients’ safety is a top priority, Professor Praditpornsilpa emphasized that the approval process for biosimilars in Thailand needs to include intensive scientific regulation. The regulatory pathway for similar biological drugs must be designed to assess quality, characterization and the impurity profile of such products, including head-to-head evaluation with a reference biological product, followed by careful head-to-head evaluation of the non-clinical and clinical aspects. Pharmacovigilance studies should be the final step to ensure quality and safety and this can be assessed together with the cost-effectiveness and patient benefits that such products offer. Professor Praditpornsilpa concluded that, in light of the issues encountered with the use of biocopy r-HuEPO in Thailand, individual case-by-case review and approval of biocopy products is needed.
Re-evaluating erythropoietin’s in Thailand
Mr Pramote Akarapanon, Head of Biological Products Section at the Ministry of Public Health, Thailand, gave a presentation entitled, ‘Experience of re-evaluating erythropoietin in Thailand’. Here, he noted that in Thailand, erythropoiesis stimulating agent EPO’s have been used for the standard treatment of anaemia in patients with chronic kidney disease for some time. However, as mentioned in Professor Praditpornsilpa’s presentation, this was associated with a high prevalence of PRCA. As a result, a re-evaluation of marketed EPO’s was instigated by a Ministerial Order, whereby the importer or manufacturer of EPO is required to submit additional data (quality, non-clinical, clinical) to the Thai Food and Drug Administration (TFDA), together with a Risk Management Plan (RMP). There are two types of RMP depending on the extent of documentation already submitted for each individual product. Mr Akarapanon noted that close monitoring of RMP’s is a big challenge for TFDA.
Following the speakers presentations, there was the opportunity for discussion of the topics covered. Herein, Dr Niklas Ekman, member of the Biosimilar Medicinal Products Working Party (BMWP) of the European Medicines Agency (EMA), made it clear that EMA only evaluates biosimilars for biosimilarity, and does not evaluate the interchangeability between a biosimilar and reference product. According to the European definition, interchangeability refers to the possibility of exchanging one medicine for another medicine that is expected to have the same clinical effect [6]. He noted that interchangeability is a national concern and is to be dealt with by individual medicines regulatory agencies of the European Union Member States, most of which have published their own position papers or statements on interchangeability that are in general, aligned. He stressed that in Europe, interchangeability means that it is the prescriber that can choose between the originator and the biosimilar, but currently there is no pharmacy-level substitution.
When it comes to switching between an originator and biosimilar, Dr Giezen advised that in Europe EMA, does not require switching studies which is in contrast to the requirements of the US Food and Drug Administration (FDA). In Europe, if a biosimilar is approved it is up to the Member States to decide on interchangeability and switching, not EMA. In general, if a biosimilar and the reference product have been shown to be similar through quality characterization and this confirmed by clinical trials, they can be switched safely and efficaciously. As such, switching studies are not necessary, and are generally only carried out to provide data to show clinicians that switching is safe. Dr Giezen added that switching studies generally have limitations, particularly if the number of patients in the study is small and adverse effects are rare. The design of switching studies and the length of time over which they are carried out, also needs to be considered.
The discussion steered towards understanding how many batches of reference product are needed to establish the Quality Target Product Profile (QTPP) of a biosimilar. Here, Dr Ekman noted that the exact number of batches is not specified by EMA requirements. However, companies are recommended to analyze reference product batches over a relatively long period of time as this means that batch-to-batch variability is better understood. Furthermore, it is in the company’s interest to analyse a reasonable number of batches of the reference product as with a small number of batches the variability present in the quality attribute of the reference product cannot be appropriately estimated. Depending on the quality attribute in question, this can result in analyses of 20 or more reference product batches.
Dr Ekman explained that for evaluating biosimilarity, orthogonal analytical methods should be used whenever possible. If only one method is applied for analysing a certain quality attribute this will usually add more burden on the qualification of the method. It needs to be demonstrated with high confidence that such a method is sensitive and can reliably detect minor differences between the originator and biosimilar. The use of orthogonal methods will increase trust in the biosimilar assessment. Speaker Dr Sundar Ramanan added that, in the case of glycosylation, it is very important to know what kind of enzyme reagents are used in the analysis and that it is critical to assess whether the results obtained from using these enzymes and subsequent separation methods, have the required sensitivity needed for adequate assessment.
In follow up to this, a question was asked about the charge variant analysis that should take place when evaluating a biosimilar. In response, Dr Ekman noted that differences in the charge variant often mean that there are differences between the originator and the biosimilar and it is critical to understand why these differences occur. After this, a more detailed discussion on charge variants and isoforms ensued.
During Professor Praditpornsilpa’s presentation he noted that while investigating r-HuEPOs, his research group encountered a cold chain and storage problem early on in their research. However, when they carried out their pharmacovigilance study, they made sure that the cold chain and storage problem did not interfere with their results. Professor Praditpornsilpa noted that, on inspection of their analytical data, although the human serum albumin was a better stabilizer compared to polysorbate 80, the purity of human serum albumin could be an issue for product quality. This highlights the fact that the quality of the preservation of a biological is key. Professor Praditpornsilpa also noted that he is skeptical about the quality of human serum albumin currently used in the biocopy EPOs in Thailand. He suspects that there may be some contamination but notes that carrying out analysis to confirm this is complicated. The analysis of the products by mass spectroscopy identified other human proteins and also rodent protein contamination. The human proteins could be related to the purity of human serum albumin for preservation and the rodent protein could be related to the separation of r-HuEPO from the cell culture. With regards to the immunogenicity occurring in Thailand that has led to 30 cases of PRCA in 2016, Professor Praditpornsilpa confirmed that this mostly occurred when biocopy products were used, rather than with originator products (although 1−2 cases per year are seen with originator products). He and his team believe that this issue is caused by protein aggregation and impurity of products.
Mr Pramote Akarapanon’s presentation also focused on PRCA occurring following EPO use. Due to the safety concerns surrounding this form of medication in Thailand, he noted that products associated with causing PRCA should be withdrawn from the market. However, during the discussion, Mr Akarapanon noted that there are no specific set timelines in place for product withdrawal and that products were being assessed on a case-by-case basis. In contrast, WHO Guideline on the reassessment of approved rDNA-derived biotherapeutics proposes a stepwise approach which includes timelines for undertaking the exercise. He also added that the public were aware of the safety concerns and of the fact that EPO products are under review.
Case study working sessions took place following the presentations (downloadable from the GaBI website [1]). These followed the same format as those described in [2–4], of two fictional cases of a follow-on biological therapeutic, one an erythropoietin product and the other a monoclonal antibody. The participants were divided into four discussion groups, see Table 1, where they evaluated the fictional data supplied. The group discussions are summarized in Tables 2 and 3.
Biosimilar medicines are being increasingly developed and used across Southeast Asia. Safety and efficacy issues that have surrounded the use of biocopy EPO’s in Thailand highlight the need for adequate evaluation and regulation of biosimilars across the region. The ASEAN Educational Workshop on Regulation and Approval of Biosimilars/Similar Biotherapeutic Products was successful in bringing representatives from ASEAN nations together with those from Europe and the US, to discuss the best routes forward for successful biosimilar approval, regulation and market introduction.
Speakers
Pramote Akarapanon, BSc Pharm, MA, Thailand
Niklas Ekman, PhD, Finland
Thijs J Giezen, PharmD, MSc, PhD, The Netherlands
Elwyn Griffiths, PhD, DSc, UK
Professor Andrea Laslop, MD, Austria
Professor Kearkiat Praditpornsilpa, MD, Thailand
Sundar Ramanan, PhD, USA
Robin Thorpe, PhD, FRCPath, UK
Meenu Wadhwa, PhD, UK
Moderators
Agnes Chan, Singapore
Azizah Ab Ghani, PhD, Malaysia
Associate Professor Maneewan Suksomtip, PhD, Thailand
Assistant Professor Wisit Tangkeangsirisin, PhD, Thailand
Editor’s comment
All moderators had provided the discussion/conclusion of the group discussion, read the report and revised the content of the summary discussion.
Acknowledgement
The Generics and Biosimilars Initiative (GaBI) wishes to thank Ms Sylvia Laksmi Sardy and Ms B Lusia Herwahyu S from the ASEAN Secretariat for their support towards the coordination of the workshop with ASEAN member states; Dr Tankamol Chanprapap, Ms Charunee Krisanaphan and Mr Pramote Akarapanon of Thai FDA for their strong support through the offering of advice and information towards the preparation and organization of the workshop; the moderators in clarifying the information of the case study discussion when finalizing the meeting report; as well as Dr Robin Thorpe and Professor Andrea Laslop, chair and co-chair of the 2017 workshop; for their strong support through the offering of advice and information during the preparation of the workshop.
The authors would like to acknowledge the help of all the workshop speaker faculty and participants, each of whom contributed to the success of the workshop and the content of this report, as well as the support of the moderators and co-moderators: Ms Agnes Chan, Dr Azizah Ab Ghani, Associate Professor Maneewan Suksomtip and Assistant Professor Wisit Tangkeangsirisin in facilitating meaningful discussion during the parallel case study working sessions, presenting the discussion findings at the workshop, and contributing in the finalization of this meeting report.
Lastly, the authors wish to thank Ms Alice Rolandini Jensen, GaBI Journal Editor, in preparing and finalizing this meeting report manuscript and providing English editing support on the group summaries.
Competing interests: The workshop was sponsored by an unrestricted educational grant to GaBI from Amgen Inc.
Provenance and peer review: Not commissioned; externally peer reviewed.
Robin Thorpe, PhD, FRCPath, UK
Elwyn Griffiths, PhD, DSc, UK
Niklas Ekman, PhD, Finland
*Biocopy refers to a licensed product made as a copy of an original product but not licensed according to the now accepted international norms of a biosimilar.
References
1. Generics and Biosimilars Initiative. First ASEAN Educational Workshop on Regulation and Approval of Biosimilars/Similar Biotherapeutic Products 2017. 23 July 2017; Bangkok, Thailand. Available from: www.gabi-journal.net/about-gabi/educational-workshops/first-asean-educational-workshop-on-regulation-and-approval-of-biosimilarssimilar-biotherapeutic-products-2017
2. Walson P, Thorpe R. First Latin American educational workshop on similar biotherapeutic products, Mexico City, Mexico, 20 January 2015. Generics and Biosimilars Initiative Journal (GaBI Journal). 2015;4(3):143-8. doi:10.5639/gabij.2015.0403.031
3. Walson P, Thorpe R. First MENA educational workshop on regulation and approval of similar biotherapeutic products/biosimilars, Dubai, United Arab Emirates, 1 September 2015. Generics and Biosimilars Initiative Journal (GaBI Journal). 2015;4(4):173-7. doi:10.5639/gabij.2015.0404.039
4. First Turkish interactive workshop on regulation and approval of similar biotherapeutic products/biosimilars 2016. Generics and Biosimilars Initiative Journal (GaBI Journal). 2016;5(3):134-8. doi:10.5639/gabij.2016.0503.034
5. Roundtable on biosimilars with European regulators and medical societies, Brussels, Belgium, 12 January 2016. Generics and Biosimilars Initiative Journal (GaBI Journal). 2016;5(2):74-83. doi:10.5639/gabij. 2016.0502.019
6. European Medicines Agency. European Commission, Biosimilars in the EU. Information guide for healthcare professionals [homepage on the Internet]. [cited 2018 Jul 12]. Available from: http://www.ema.europa.eu/docs/en_GB/document_library/Leaflet/2017/05/WC500226648.pdf
|
Author for correspondence: Robin Thorpe, PhD, FRCPath, Deputy Editor-in-Chief, GaBI Journal |
Disclosure of Conflict of Interest Statement is available upon request.
Copyright © 2018 Pro Pharma Communications International
Permission granted to reproduce for personal and non-commercial use only. All other reproduction, copy or reprinting of all or part of any ‘Content’ found on this website is strictly prohibited without the prior consent of the publisher. Contact the publisher to obtain permission before redistributing.
Source URL: https://gabi-journal.net/first-asean-educational-workshop-on-regulation-and-approval-of-biosimilars-similar-biotherapeutic-products-2017-report.html
|
Abstract: |
Submitted: 7 February 2018; Revised: 8 May 2018; Accepted: 9 May 2018; Published online first: 22 May 2018
Similar Biotherapeutic Products (SBPs or biosimilars) have emerged as a new class of biotherapeutic agent. They are being increasingly developed and are becoming more available worldwide. However, approaches to how they are regulated vary across the world. The European Union (EU) has successfully pioneered regulatory procedures and has over 10 years of experience in the regulation and approval of biosimilars. In light of this, other countries across the globe are turning to regulatory experts from Europe and the US for advice on how best to conduct quality assessment of biologicals/biosimilars, to ensure that safety and efficacy of treatment is upheld.
To facilitate discussion concerning quality assessment of biologicals/biosimilars in Colombia, the Generics and Biosimilars Initiative (GaBI) organized an educational workshop [1] and a follow-up meeting [2] in collaboration with the National Food and Drug Surveillance Institute of Colombia (Instituto Nacional de Vigilancia de Medicamentos y Alimentos, INVIMA), in 2016 and 2017 respectively. Presentations were made by both international speakers, as well as regulators from Colombia.
The First INVIMA Educational Workshop on the Assessment of Similar Biotherapeutic Products [1] was an interactive event held on 14 June 2016. The format used was similar to that used in prior educational workshops as reported in GaBI Journal [3, 4]. More details of the methods and case presentations can be found in the published reports of the First Latin American Educational Workshop on Similar Biotherapeutic Products [3] and the First MENA Educational Workshop on Regulation and Approval of Similar Biotherapeutic Products/Biosimilars [4]. Summaries of the presentations that were given on analytical comparability, clinical and non-clinical assessment, and safety assessment, are available in the published reports of the Roundtable on biosimilars with European regulators and medical societies [5].
The Second Colombian Scientific Meeting on Quality Assessment of Biosimilars/Similar Biotherapeutic Products [2] was held on 15 August 2017, and focussed on the key topics of: comparability of production processes, design and execution of analytical comparability studies/forced degradation studies, analytical methods, preparation and production of reference standards, and development and validation of host cell protein assays, with a keynote presentation on the Norwegian NOR-SWITCH study on the replacement from originator product to biosimilar infliximab. The meeting was chaired by Dr Elaine Gray and Dr Paul Matejtschuk, who are both Principal Scientists at the UK’s National Institute for Biological Standards and Control (NIBSC).
Both Colombian meetings were held in Bogotá. The list of speakers and the slides they presented are available on the GaBI Journal website (www.gabi-journal.net/about-gabi/educational-workshops).
In addition to the expert presentations as delivered in prior meetings [3–5], Dr Elwyn Griffiths, former Director General of the Biologics and Genetic Therapies Directorate, Health Canada, gave a presentation entitled ‘Regulatory assessment of already approved rDNA-derived biotherapeutics’, which was an update to that given at the First Turkish Interactive Workshop on Regulation and Approval of Similar Biotherapeutic Products/Biosimilars [4]. He highlighted the role of the World Health Organization (WHO) to ensure global harmonization and regulation of rDNA-derived biotherapeutics. He also summarized the issues they have encountered in implementation, particularly related to products already approved prior to the development of regulatory processes. He introduced the WHO’s new guideline for stepwise product specific regulatory assessment and highlighted the WHO document on regulatory assessment on rDNA derived biotherapeutics.
Initially, a query was raised on whether clinical data is required when a manufacturing process is scaled up; with a simple linear up-scaling of a process it was considered that clinical data is not generally required but if there are procedural changes, then such data may be required and comparability cannot be assumed. Currently, for a biosimilar to be approved, clinical data must be supplied to support biosimilarity.
When asked if small biologicals approved without clinical studies, could be termed biosimilars, it was noted that this had not been done in Europe nor in the US. It was explained that, in biosimilar production, a biosimilar does not need to be manufactured using the same expression system as the reference biological and, in practice, using the exact same system would be impossible. However, the manufacturing process must produce an active substance sufficiently similar to that produced by the originator manufacturer. When developing a biosimilar, companies create a database based on a relatively large number of reference batches in order to have sufficient information on the reference product to produce their own Quality Target Product Profile (QTPP). This is not directly required by regulators, but such data is needed to ensure product comparability.
Regarding compiling comparability data, the biosimilar manufacturer must also produce data on the reference product at the same time as producing data on the biosimilar. This data is not readily available and, although some results relating to originator products are published on occasion, these should always be reproduced and made available by the biosimilar manufacturer in order for them to undertake comparability studies. For clinical comparison, pharmacokinetic (PK) and pharmacodynamic (PD) comparisons are a minimum requirement for authorization of biosimilars and in addition, a clinical assessment of the immunogenicity.
Case study working sessions took place following the presentations (downloadable from the GaBI website [1]). These followed the same format as those described in previous workshops [3, 4, 6], where two fictional cases of follow-on biological therapeutics are described, one an erythropoietin product and the other a monoclonal antibody. The participants were divided into discussion groups where they evaluated the fictional data supplied. The group discussions are summarized in Tables 1 and 2.
The 2017 meeting began with Welcoming Remarks by Mr Javier Humberto Guzmán Cruz, Director General of INVIMA, who gave a short presentation on the current development of INVIMA and the health system in Colombia.
The presentation began with an outline of the progress made in Colombia in the last 25 years in terms of universal health coverage. Mr Guzmán noted that Colombia is now in the process of entering the Organisation for Economic Co-operation and Development (OECD). As part of this, experts visited Colombia and carried out a review of Colombia’s health system in which they stated that, ‘Colombia has a well-designed health system, with broadly effective policies and institutions that other countries could learn from and that deserves to be better known internationally’. However, he added that the health system in Colombia is fragile and needs to remain sustainable. To ensure this, pharmaceutical policy needs to be kept up-to-date and innovations incorporated in a controlled manner to guarantee access to safe and efficacious products. Here, Mr Guzmán noted that INVIMA can have an important role in influencing pharmaceutical policy.
INVIMA was created in 1993, and the institute became officially established in 1995, following the passing of a law that aimed to achieve healthcare reform. It has grown substantially in 25 years and now has a budget of US$48 million and many facilities. However, INVIMA faces challenges in the coming years, particularly those posed by the entry of products from large pharmaceutical manufacturers to the Colombian market. Regulators and the Colombian health system need to do work on deciding what gets included in the market to enable the development of frameworks that encourage competition to create access to generics and biosimilars. Mr Guzmán stated that, in Colombia, improving competition that guarantees quality, safety and efficacy is more important than regulation of the pricing of therapeutics. In the last seven years, no biosimilars have been approved, as the guidelines for regulatory approval were not yet developed. Now that the regulations on biologicals/biosimilars are in place, the next challenge is effective implementation. INVIMA has the role of implementing the new regulation on biologicals/biosimilars, and staff are trained both internally and abroad to implement this new legislation. Nonetheless, they are keen to receive advice from those in Europe and the US, who have useful experience in implementation of similar regulations.
Following the Welcoming Remarks, a series of additional presentations were given by experts from Europe and the US (presentations downloadable from the GaBI website [2]). A full manuscript on the presentation of ‘Biosimilar regulations in Colombia,’ is published in GaBI Journal [7]; and information about the presentation entitled ‘Switching from originator products to biosimilars in rheumatology, dermatology and gastroenterology: clinical evidence,’ which described the NOR-SWITCH study, is also published in GaBI Journal [8].
Discussion following ‘Biosimilar regulations in Colombia’
Dr Gray asked if Colombia expects that a national pharmaceutical company would attempt to register for the three different pathways for products in the future, either via the complete dossier, comparability, and abbreviated comparability approach. Ms Garcia responded that currently, Colombia does not yet have laboratories that will submit information to comply with the new regulations as they have not yet been implemented, however, there are interests from multinational companies to support this requirement.
Discussion following ‘Switching from originator products to biosimilars in rheumatology, dermatology and gastroenterology: clinical evidence’
Professor Tore Kristian Kvien was asked about the results obtained in the switching clinical trials in Scandinavian populations and to what extent these results can be extrapolated to populations, such as the Colombian population. He stated that, in terms of efficacy, there should be no concern using the data with another population and that the NOR-SWITCH data can be used in Colombia.
With regard to patients whose treatment was switched to the Remsima biosimilar and whose disease then worsened, Professor Kvien noted that all patients were followed for one year, and those whose condition worsened also received additional treatment. If they had progression of their disease that required some change in therapy, then they were switched to another biological agent and no patients received the originator Remicade.
In relation to pharmacovigilance data, Professor Kvien noted that this was not part of the NOR-SWITCH study because it was a randomized clinical trial. However, he added that, in Norway, there is a registry called the NOR-DMARD, the Norwegian Antirheumatic Drug Register, and that the data from NOR-DMARD was also examined regarding patients who started with the biosimilar infliximab and patients who have switched from Remicade to Remsima. There does not seem to be any major concern with regards to differences in pharmacovigilance data. Despite this, he noted that the data from NOR-DMARD are not as robust as the data from DANBIO (the nationwide registry for biological therapies in Denmark), which includes some pharmacovigilance data which also support switching.
When asked if he thinks clinical trials are absolutely necessary to confirm efficacy and safety of a biosimilar agent, Professor Kvien said there is a general agreement that, with the current regulations, preclinical quality data need to be generated which support biosimilarity, but this needs confirmation using clinical studies (as outlined in his presentation for CT-P13 and SB4) [8]. Regarding whether or not a NOR-SWITCH study for every biosimilar is needed, another randomized switch study may be required. He gave the example of adalimumab, which is in need of this as it is also immunogenetic. However, it may not be feasible to perform a blinded controlled study of switching from an originator to a biosimilar self-administered drug.
Given the progress in Norway with the adoption of biosimilars, Professor Kvien noted that they would continue on the current path and introduce more biosimilars as they enter the market. The annual tender system means that the system is very competitive which leads to lower prices for the different biosimilars, and the originator products. Regarding his advice for Colombia, he thinks that in general, transparency and competition is important. It is also important that regulators collaborate with key opinion leaders and experts in the different clinical disciplines, so that there are alliances with the clinical environment, which will help to implement the use of biosimilars in Colombia.
Discussion following ‘Preparation and production of reference standards in support of biotechnology products’
Dr Matejtschuk was asked about secondary standards and what they are used for. He said that a secondary standard might be a pharmacopoeial standard and gave the example of a standard from the United States Pharmacopeia (USP) or European Directorate for the Quality of Medicines & HealthCare (EDQM). This will not usually be a primary standard as the dose is not defined, but will actually be a secondary reference material. He noted that working standards could also be secondary standards. Dr Gray added that the WHO International Standards (IS) are primary standards and as such are produced infrequently with a substantial international collaboration required to assign values, and their usage is carefully controlled to maintain stocks and ensure continuity. Pharmacopoeial, regional, working or in-house standards are secondary standards, calibrated against the IS.
Discussion following ‘Value assignment of International Standards: challenges for potency labelling of biotechnology/biosimilar products’
There was a question about reference units, standards and dosing. Dr Gray said that, for a product such as a monoclonal antibody, which is already dosed in milligrams, there would be no attempt to change the dosing to arbitrary units. So, the activity in terms of the international unit is really for the control of the bioassay, this does not impact on the dosing and potency labelling of these products. The aim of such standards would be to aid manufacturers in monitoring consistency of production. For other biological products that do label potency in international units, such as for the coagulation factors, the continuity of the unit is ensured by calibrating against the existing standard, in order to have traceability of the unit each time a replacement standard is made. However, some slight variability is inevitable because batches of such materials are unique, and there may be some drift in potency depending on the assay and the materials themselves.
Colombia’s health service has improved greatly over the past 25 years and standards of heath care and access to treatments are high. Over the last seven years the country has been developing a regulatory framework to allow biosimilar products to enter the market and Colombia is now at a point where it can start implementing regulatory approval policy for biologicals/biosimilars. The educational workshop and the scientific meeting created a platform for those involved with biological/biosimilar regulation in Colombia to meet with experts from Europe and the US and a number of interactive discussions took place. The attendees shared ideas with the speakers and received clarification on issues of interest and concern.
Speakers
2016 Educational Workshop
Niklas Ekman, PhD, Finland
Thijs J Giezen, PharmD, MSc, PhD, The Netherlands
Gustavo Grampp, PhD, USA
Elwyn Griffiths, DSc, PhD, UK
Professor Andrea Laslop, MD, Austria
Robin Thorpe, PhD, FRCPath, UK
2017 Scientific Meeting
Johanna Andrea Garcia Cortes, MSc, Colombia
Elaine Gray, PhD, UK
Professor Tore Kristian Kvien, MD, Norway
Jennifer Liu, PhD, USA
Paul Matejtschuk, PhD, CChem, UK
Sundar Ramanan, PhD, USA
Moderators and Co-moderators
2016 Educational Workshop
Jeannette Daza Castillo
Andrey Forero Espinosa
Angélica Fula Arguello
Diego Alejandro Gutierrez Triana
Inés Elvira Ordoñez
Claudia Yaneth Niño C
The Generics and Biosimilars Initiative (GaBI) wishes to thank Dr Robin Thorpe and Professor Andrea Laslop, chair and co-chair of the 2016 workshop; and Dr Elaine Gray and Dr Paul Matejtschuk, chair and co-chair of the 2017 meeting; for their strong support through the offering of advice and information during the preparation of the workshop and meeting, respectively. Further, GaBI wishes to thank Mr Francisco Javier Sierra Esteban of INVIMA for his feedback and comments on this Meeting Report.
The authors would like to acknowledge the help of all the workshop and meeting speaker faculty and participants, each of whom contributed to the success of the workshop and meeting and the content of this report, as well as the support of the moderators and co-moderators for the 2016 workshop: Jeannette Daza Castillo, Andrey Forero Espinosa, Angélica Fula Arguello, Diego Alejandro Gutierrez Triana, Inés Elvira Ordoñez, Claudia Yaneth Niño C, in facilitating meaningful discussion during the parallel group discussions; and presenting the discussion findings at the 2016 workshop.
Lastly, the authors wish to thank Ms Alice Rolandini Jensen, GaBI Journal Editor, in preparing this meeting report manuscript and providing English editing support on the group summaries and for finalizing this manuscript.
Competing interests: The workshop and meeting were sponsored by an unrestricted educational grant to GaBI from Amgen Inc.
Provenance and peer review: Not commissioned; externally peer reviewed.
Elaine Gray, PhD
Principal Scientist, Haemostasis Section Biotherapeutics Group
Paul Matejtschuk, PhD, CChem
Principal Scientist – Standardisation Science
National Institute for Biological Standards and Control (NIBSC), Blanche Lane, South Mimms, Potters Bar, Hertfordshire EN6 3QG, UK
Robin Thorpe, PhD, FRCPath
Deputy Editor-in-Chief, GaBI Journal
References
1. Generics and Biosimilars Initiative. First INVIMA Educational Workshop on Assessment of Similar Biotherapeutic Products 2016; 14 June 2016; Bogotá, Colombia. Available from: www.gabi-journal.net/about-gabi/educational-workshops/first-invima-educational-workshop-on-assessment-of-similar-biotherapeutic-products-2016
2. Generics and Biosimilars Initiative. Second Colombian Scientific Meeting on Quality Assessment of Biosimilars/Similar Biotherapeutic Products 2017; 15 August 2017; Bogotá, Colombia. Available from: www.gabi-journal.net/second-colombian-scientific-meeting-on-quality-assessment-of-biosimilarssimilar-biotherapeutic-products-2017
3. Generics and Biosimilars Initiative. First Latin American educational workshop on similar biotherapeutic products; 20 January 2015; Mexico City, Mexico. Available from: www.gabi-journal.net/first-latin-american-educational-workshop-on-similar-biotherapeutic-products-mexico-city-mexico-20-january-2015.html
4. Walson PD, Thorpe R. First MENA educational workshop on regulation and approval of similar biotherapeutic products/biosimilars, Dubai, United Arab Emirates, 1 September 2015. Generics and Biosimilars Initiative Journal (GaBI Journal). 2015;4(4):173–7. doi:10.5639/gabij.2015.0404.039
5. Annese V, Avendaño-Solá C, Breedveld F, Ekman N, Giezen TJ, MSc, Gomollón F. Roundtable on biosimilars with European regulators and medical societies, Brussels, Belgium, 12 January 2016. Generics and Biosimilars Initiative Journal (GaBI Journal). 2016;5(2):74–83. doi:10.5639/gabij.2016.0502.019
6. Walson PD, Thorpe R. First Turkish interactive workshop on regulation and approval of similar biotherapeutic products/biosimilars, 2–3 March 2016, Ankara, Turkey. Generics and Biosimilars Initiative Journal (GaBI Journal). 2016;5(3):134–8. doi:10.5639/gabij.2016.0503.034
7. García Cortes JA, Sierra Esteban FJ. Regulations for biotherapeutics approval in Colombia. Generics and Biosimilars Initiative Journal (GaBI Journal). 2018;7(1):26-8. doi:10.5639/gabij.2018.0701.006
8. Perks B. Randomized non-inferiority trial fails to find inferiority switching from infliximab originator to CT-P13 biosimilar. Generics and Biosimilars Initiative Journal (GaBI Journal). 2017;6(4):188-9. doi:10.5639/gabij.2017.0604.042
|
Author for correspondence: Robin Thorpe, PhD, FRCPath, Deputy Editor-in-Chief, GaBI Journal |
Disclosure of Conflict of Interest Statement is available upon request.
Copyright © 2018 Pro Pharma Communications International
Permission granted to reproduce for personal and non-commercial use only. All other reproduction, copy or reprinting of all or part of any ‘Content’ found on this website is strictly prohibited without the prior consent of the publisher. Contact the publisher to obtain permission before redistributing.
Source URL: https://gabi-journal.net/quality-assessment-of-biosimilars-in-colombia-reducing-knowledge-gaps.html
Author byline as per print journal: Professor Francisco José de Abajo, MD, MPH, PhD; Professor Joan Albanell, MD; Olga Delgado Sanchez, PharmD; Kevin Klein, MSc; José Vicente Moreno-Muelas, MD; Sol Ruiz, PhD; Professor Maria Jesús Sanz Ferrando, PhD; Robin Thorpe, PhD, FRCPath; Professor Francisco Zaragozá, PhD
|
Introduction: Biosimilars can offer a lower-cost alternative to current biological therapies and could help contribute to the much-needed savings for the healthcare systems. All biosimilars approved by the regulators must show comparable efficacy and safety with the reference biologic. However, the acceptance by the healthcare professionals and by patients is not uniform within Europe. Therefore, it is important to understand the barriers to biosimilar uptake. Increased awareness amongst the stakeholders – regulators, prescribing physicians, medical societies, pharmacists and patients – to the barriers and plausible solutions could help improve further uptake of biosimilars. |
Submitted: 2 February 2017; Revised: 25 February 2017; Accepted: 27 February 2017; Published online first: 3 March 2017
Biosimilars offer a prospect of savings to the health systems given they are generally priced lower than the reference product. The uptake of biosimilars across Europe has not been uniform across all countries. The challenges posed by biosimilars – which are different versions of the innovator biological medicines on which they are based – are viewed in different ways. Biosimilar uptake has been relatively slow in Spain, where physicians do not appear to be readily in favour of the extrapolation of indications, despite guidance otherwise from the European Medicines Agency (EMA). There are also concerns around the effectiveness of current pharmacovigilance systems.
The Generics and Biosimilars Initiative (GaBI), with its mission to foster the worldwide efficient use of high quality and safe medicines at an affordable price, organized a roundtable discussion on biosimilars (focussing on pharmacovigilance, traceability and immunogenicity) for Spanish physicians, pharmacists and medical societies. The aim of the meeting was to learn about the challenges faced in Spain as a steadily growing number of biosimilars are approved and enter the European market.
The main themes of the meeting were on the practical challenges in the implementation of robust pharmacovigilance systems; and how to establish pharmacovigilance schemes to enhance traceability and post-marketing surveillance of biologicals including biosimilars.
The meeting was organized in collaboration with the Faculty of Medicine and Pharmacy of the University of Alcalá, and chaired by Professor Francisco Zaragozá, past-president of both the Spanish Society for Pharmacology and the European Pharmaceutical Advisory Committee. He is currently Professor of Pharmacology at the Faculty of Medicine and Pharmacy, University of Alcalá, Madrid, Spain.
Presentations were made by European speakers as well as local academic faculty, clinicians, pharmacists and Spanish regulators. The list of speakers and panel members is detailed at the end of this report, and all speakers’ presentations are available on the GaBI Journal website (www.gabi-journal.net/about-gabi/educational-workshops).
On 15 November 2016, GaBI held a Roundtable on Biosimilars in Madrid, Spain, with participation by physicians and pharmacists from Spain, as well as other experts from Europe. The programme offered speaker presentations and a discussion session to provide participants with current views on biosimilars in Spain. Presentations were in Spanish or English (with simultaneous translation).
Biological medicines
The Roundtable was opened by the Chair, Francisco Zaragozá, Professor of Pharmacology at the Faculty of Medicine and Pharmacy, University of Alcalá, Madrid, Spain. Professor Zaragozá gave an overview of biological medicines including biosimilars, covering both the promise and the concerns that surround these therapies. The greatest promise of biosimilars is that they will drive down healthcare costs, both in terms of the cost of treatment and the savings made by cutting hospital readmissions. But are the concerns justified?
The introduction of therapeutic monoclonal antibodies, such as infliximab, was a notable milestone. Two biosimilars of infliximab (Inflectra and Remsima) were approved by EMA in 2013, and Inflectra was approved by the US Food and Drug Administration (FDA) in 2016.
Unlike generics which have the same active ingredient as the reference drug, the structural differences between the biosimilars and the reference biological was a concern for Professor Zaragozá. Thus, ‘We need to be very cautious in our approach’ in the use of biosimilars, he warned, calling on regulators to improve communication by providing more clarity on their rationale for the decisions.
EMA approval requirements on biosimilars: clinical aspects
Dr Sol Ruiz, Head of Biotechnology and Advanced Therapies at the Spanish Agency for Medicines and Medical Devices (Agencia Española de Medicamentos y Productos Sanitarios) and chair of EMA’s Biologics Working Party, discussed the quality and clinical aspects of EMA approval requirements for biosimilars. Dr Ruiz began by presenting a list of all biosimilars approved by EMA to date [1], demonstrating that the number of biosimilars is increasing year-over-year.
The procedure of establishing biosimilarity is a step-wise process that can be split into three categories: extensive characterization (of physicochemical structure and biological activity); in vitro functional activity (analysing all possible modes of action [MoA] of the molecule); and efficacy and safety studies (using the most sensitive or relevant population to detect differences).
Biosimilarity from a clinical perspective starts by showing a comparable pharmacokinetic (PK) profile in a sufficiently sensitive and homogeneous population of healthy volunteers, if possible. For pharmacodynamic (PD) studies, the use of multiple PD markers is recommended if possible. PD markers can be used as pivotal evidence for comparable efficacy if a clear dose-response relationship is shown, and if at least one PD marker is an accepted surrogate for efficacy, i.e. can be related to patient outcome.
Comparative studies looking at efficacy and safety must by adequately powered, randomized, preferably double blind and are normally equivalence trials. Any deviation from relevant efficacy guidelines should be justified. For these studies, usually the most sensitive patient population is preferred.
Dr Ruiz summarized the clinical studies carried out to establish the biosimilarity of CT-P13 (Remsima) with its innovator infliximab. In June 2013, CT-P13 (with the brand names Remsima [Hospira] and Inflectra [Celltrion]) were recommended for approval by EMA’s Committee for Medicinal Products for Human Use (CHMP) and is available in the European Union (EU). Inflectra was subsequently approved by FDA in April 2016, following a submission by Celltrion and its partner Pfizer.
Extrapolation of indications continues to be the most controversial issue affecting the uptake of biosimilars, said Dr Ruiz. As the list of approved biosimilars grows, regulators should make the effort to better communicate the reasoning behind the decisions made.
Evaluation of immunogenicity of biosimilars
Dr Robin Thorpe, former head of the Biotherapeutic Group at the UK’s National Institute for Biological Standards and Control, spoke about the issue of unwanted immunogenicity of biological medicines. Immunogenicity can have significant clinical consequences leading to reduced clinical efficacy, hypersensitivity or allergic reactions. Immunogenicity assessment is a vital component of regulatory submissions for product approval.
Immunogenicity assessment requires carefully planned prospective studies in a suitable indication, a well-considered strategy and a panel of appropriately validated assays for antibody detection and characterization in clinical samples. Determining the immunogenicity of biosimilar products requires similar assessment approaches to stand-alone products, but in addition comparative immunogenicity studies with the reference product are required.
Biological products can induce antibodies with different characteristics and different assays are needed to detect and measure these antibody types.
Dr Thorpe made clear that there was no reason to treat approved biosimilars any differently from all biologicals from the immunogenicity perspective. He presented data from European public assessment reports (EPARs) showing antibody frequencies for biosimilars and their reference products. Clearly neither group – biosimilar nor reference – routinely has a higher or lower antibody frequency, see Table 1.
Immunogenicity is a serious and challenging issue. It is impossible to predict when it will happen and what clinical consequences it will have. Appropriate studies are clearly needed to assess such risks. It is important to remember that immunogenicity is not new or specific to biological therapies – it exists ‘for just about everything’, said Dr Thorpe.
The factors that influence unwanted immunogenicity are shown in Box 1.
Current guidance from EMA, FDA and World Health Organization (WHO) stipulates that testing for unwanted immunogenicity is integral to product development, that animal data is not predictive of immunogenicity in humans, and that every product needs to be evaluated for immunogenicity individually and an appropriate strategy adopted based on intended clinical use. Dr Thorpe noted that EMA’s CHMP guidelines are about to be updated.
There is no perfect assay for antibody testing. CHMP recommends a tiered approach to immunogenicity testing: starting with screening assays (to identify anti-therapeutic antibodies); followed by confirmatory assays; and finally neutralization assays (to discriminate between neutralizing and non-neutralizing antibodies, see Figure 1.
Even though immunogenicity assessment strategy needs to be established on a case-by-case basis (product, patient, expected clinical parameters), unwanted immunogenicity always remains a possibility. Immunogenicity can arise throughout a product’s life cycle. In addition to this, post-approval assessment, as part of pharmacological surveillance, is key.
Understanding pharmacovigilance for biologicals and the current challenges in Spain
Francisco José de Abajo, Professor of Clinical Pharmacology at the University of Alcalá, Madrid, Spain began his presentation on the issue of pharmacovigilance in Spain by noting that pharmacovigilance for biological medicines is largely the same as for pharmaceuticals. Two differences, however, are that greater importance is placed on the possibility of immunogenicity, and on the impact of quality issues on safety.
Professor de Abajo reviewed a new chapter in the EMA guidelines on good pharmacovigilance practices (EU-GVP), entitled ‘Product or population specific considerations II: biological medicinal products’, which came into force in August 2016 [2]. The new chapter provides guidance on how to better monitor and manage the safety of biological medicines to optimize the safe and effective use of these products in Europe.
Professor de Abajo contrasted the classical view of pharmacovigilance, the reactive model, see Figure 2a with the current view, the proactive model, see Figure 2b.
The risk management plan, see Figure 2b, aims to anticipate potential safety issues, carry out epidemiological studies, implement risk minimization measures and check the effectiveness of measures adopted.
Biologicals require particularly stringent pharmacovigilance since they are complex molecules that are considered more likely to trigger immune reactions.
Clinical data collected from patients who have been treated with biological therapies in Spain have been included in national databases in order to identify and help predict and prevent possible adverse events. The Spanish Agency for Medicines and Medical Devices’ database BIFAP (www.bifap.org), which currently includes data from eight million patients seen by general practitioners in Spain, is similar to the UK’s Clinical Practice Research Datalink (CPRD) and The Netherlands’ IPCI (Integrated Primary Care Information). Sadly, most biological treatments are dispensed in hospitals and are not included in BIFAP or in many other pharmacoepidemiological databases.
An alternative source of information is the creation of ad hoc registries of exposed patients (treated with drugs of interest) or registries of cases (patients with the disease or event of interest). An example of the former in Spain is the BIOBADASER registry – created by the Spanish Society of Rheumatology and partially funded by the Spanish Medicines Agency and several pharmaceutical companies. BIOBADASER (https://biobadaser.ser.es) provides a registry of patients treated with biologicals for rheumatic diseases. Such a registry has been successfully used to test some pharmacovigilance signals concerning these products, either confirming them, e.g. tuberculosis associated with infliximab, or refuting them, e.g. cancer associated with these biological products. This database has included in its phase II over 7,000 patients. It has helped show the effectiveness of risk minimization measures on reducing cases of tuberculosis in patients treated with infliximab. More recently, a similar initiative has been taken by the Spanish Academy of Dermatology and Venereology (AEDV) setting up a database called BIOBADADERM, which includes patients treated with biological products for dermatological conditions, e.g. psoriasis (https://biobadaderm.fundacionpielsana.es).
Professor de Abajo says the Spanish pharmacovigilance system is well prepared for the challenge of biologicals, but complementary epidemiological approaches will improve this. BIOBADASER provides a roadmap to follow.
Current challenges in traceability of biologicals – a case study from The Netherlands
Kevin Klein, a researcher at Escher, the Lygature platform for regulatory innovation in The Netherlands, spoke about a recent pilot study he has been working on looking at pharmacovigilance of biologicals.
Klein and his colleagues evaluated information-recording systems and practices in the Dutch hospital and community setting to identify determinants for brand name and batch number recording as well as success factors and bottlenecks for traceability. His team found limited traceability of brand names and batch numbers in reports of adverse drug reactions (ADRs), which they concluded might be primarily caused by the shortcomings in the recording of information in clinical practice.
To align practice with the ambition of the EU pharmacovigilance legislation regarding traceability, brand name and batch number recording needs to be (further) improved, says Mr Klein. Additional case studies in different Member States could help to map EU differences, commonalities and potential success factors for activities/interventions to improve traceability.
Considerations of the Spanish Society of Pharmacology on pharmacovigilance, traceability and immunogenicity of biosimilars from the biomedical perspective
Maria Jesus Sanz Ferrando, President of the Spanish Society of Pharmacology and Professor of pharmacology at the University of Valencia, highlighted the Spanish Society of Pharmacology’s concerns at the level of pharmacovigilance, traceability and immunogenicity of biologicals including biosimilars, specifically monoclonal antibodies.
Professor Sanz acknowledged that the introduction of biosimilars was a great advance for Spain’s national health system, but strong pharmacovigilance that includes both health professionals (including doctors, pharmacists and nurses) and patients in the communication of efficacy and adverse reactions of all products is needed.
Further development of techniques aimed at detecting the possible immunogenicity of each product is required. The Spanish Society of Pharmacology recommends that prescription of biosimilars be made by brand name, batch number and manufacturer to enable traceability in case of adverse events. The Society holds that extrapolation to other indications without previous clinical trials will require advances in in vitro studies and more sophisticated and reliable animal models.
Antibody biosimilars in oncology: an analytical to clinical perspective
Professor Joan Albanell, member and coordinator of the Spanish Society of Medical Oncology’s Biosimilars Working Group and Professor of Oncology at Pompeu Fabra University, warned against the interchangeability of biosimilars and reference drugs without specific clinical studies on the same indication in support of its safety and efficacy.
The Spanish Society of Medical Oncology’s (SEOM) position on biosimilar monoclonal antibodies is that these drugs are unlike other biosimilars (like erythropoietin and colony stimulating factors), which have easy to measure efficacy surrogate markers, e.g. haemoglobin concentrations and leukocyte levels. The challenges posed by monoclonal antibodies, such as Trastuzumab, lie in their structural complexity, their role in the treatment of a wide range of tumours, the limited correlation between efficacy surrogate markers and clinical benefits, and the heterogeneity of their mechanisms of action.
SEOM’s position on the possibility of extrapolating from a specific trial with a homogeneous population with a clinical endpoint capable of detecting differences in activity to other indications in which the drug’s mechanisms of action, the disease biology and the treatment objectives can be different, is that it should be done only on a case-by-case basis and when the mechanism of action is clear.
Since the biosimilar and the reference biological are different drugs, argues SEOM, interchangeability should not be automatic at the time of dispensing and it can only be acceptable in certain cases, with clinical justification. The situation would be different, says Professor Albanell, if there were specific clinical studies proving the safety of interchangeability at an individual level, as regulated by FDA. However, viability of these clinical trials is difficult.
Professor Albanell noted that biosimilar manufacturers have only limited knowledge of the reference product, see Figure 3, and that monoclonal antibodies are heterogenous complex proteins that are sensitive to manufacturing conditions. For example, differences in glycosylation may lead to differences in biological function, see Figure 4.
The introduction of monoclonal antibody biosimilars in oncology is welcomed given their potential to reduce treatment costs, but their multiple, not fully understood, mechanisms of action and post-translational modifications, coupled with the complexity of cancer biology, poses a significant challenge.
SEOM agrees with the need to prescribe by brand name and, further, requires that before introducing a biosimilar in a hospital, adequate circuits be established for prescription, dispensing, administration and registration using the brand name. Pharmacovigilance of biosimilars is regulated as obligatory at a European level to rule out differences with the original biological in relation to efficacy or toxicity among the healthy population.
Position statement of the Spanish Society of Rheumatology on biosimilar drugs. Clinical vision
Dr José Vicente Moreno-Muelas, former president of the Spanish Society of rheuma-tology (SER) and faculty member at the Rheumatology Department of the University Hospital Vall d’Hebron in Barcelona, Spain welcomed the arrival of biosimilars, which have opened access to biological therapy for rheumatology patients. But, echoing concerns voiced elsewhere at this Roundtable meeting, there are several areas of concern – the issues of substitution by the hospital pharmacy, automatic switching between the innovator and the biosimilar, and the need for improved pharmacovigilance.
SER holds that the decision to prescribe a biosimilar or its innovator lies solely with the prescribing physician. The exchange of an innovator for its biosimilar is a medical act that must be performed exclusively by the prescribing physician, with the consent of the patient.
Since biosimilar drugs are subject to a safety follow-up similar to that of their reference drugs, it is necessary to create specific pharmacovigilance records. SER has extensive experience in these registries and offers to carry out these security studies.
As biosimilars currently have the same international non-proprietary name (INN) as their innovators, prescription must be made by brand name in order to achieve adequate traceability. SER states that the demonstration of efficacy and safety of a biosimilar for a given indication may not be the same as for a second indication in which the reference biological drug has demonstrated efficacy and safety. When the reference drug has more than one indication, the extrapolation of indications should be justified in accordance with EMA standards. SER argues that, if necessary, each authorized indication should be individually demonstrated with double-blind, randomized, direct comparison clinical trials with the reference drug [3]. SER’s position will be updated periodically in the light of new evidence, most likely within the next two years.
Biosimilars: something more than clinical evidence
Despite the evidence of efficacy, a solid regulatory framework and the experience of switching and safety of biosimilars, the uptake of biosimilars in European markets has been patchy, notes pharmacist Dra Olga Delgado, who heads the pharmacy department at the University Hospital Son Espases, Palma de Mallorca, Spain. Dra Delgado welcomes the introduction of biosimilars, and presented evidence of the clear benefits that increased biosimilar uptake can have on reducing the cost of treatment.
She gave examples of how uptake of biosimilars varied between hospitals in the Balearic Islands and can be lower than 10% and even down to 0% in one hospital. Dra Delgado argued that healthcare professionals clearly needed more than just evidence to implement biosimilars in practice. Her approach to this challenge is that more incentives are needed for clinicians, together with more education and support for patients, and an agreement to share the savings offered by biosimilars over their innovators. Biosimilars are an opportunity for collaboration.
The opportunities offered by biosimilars were welcomed by all speakers. Realizing these opportunities will take much open discussion and sharing of information between everyone involved in the uptake of biosimilars – prescribing physicians, medical societies, patients, pharmacists and regulators.
There was broad agreement that improved pharmacovigilance is needed. The importance of recording the brand name, as well as prescribing by brand name, was noted by the Spanish Society of Pharmacology, the Spanish Society of Rheumatology and the Spanish Society of Medical Oncology. Likewise, the importance of recording the batch number was noted by the Spanish Society of Pharmacology. Both batch number and brand name recording were highlighted by Mr Kevin Klein, whose research in The Netherlands shows that improvements in recording these details are needed in order to meet EU pharmacovigilance legislation.
The role of registries – of both patients and cases – was also raised. The Spanish Society of Rheumatology has created the BIOBADASER registry with support from the pharmaceutical industry and the Spanish Medicines Agency. This registry of patients with rheumatic diseases treated with biologicals has helped support pharmacovigilance and shown the effectiveness of risk minimization measures, for example, by reducing cases of tuberculosis in patients treated with infliximab. Similarly, the Spanish Academy of Dermatology and Venereology (AEDV) is setting up a database called BIOBADADERM for patients with dermatological diseases treated with biologicals. Risk minimization is key to the risk management plan, which lies at the heart of the currently accepted proactive model of pharmacovigilance.
The risk management plan was used to allay pharmacists’ and prescribers’ fears that they were not being made aware of any changes made to the formulation of innovator or biosimilar medicines. With a risk management plan in place, such changes will be recorded appropriately, followed closely and the information made available. Some prescribers complained that they were not told when manufacturing changes are made to biologicals.
It was clear that the authorization of biosimilars by regulatory bodies, such as EMA, does not automatically persuade prescribers to stop prescribing innovator biologicals in favour of biosimilars. A similar outcome was seen at a recent GaBI Roundtable in Brussels where regulators and physicians discussed access to biological therapies [4]. More easily accessible, clear information on the reasoning behind regulatory approvals is needed. The structural differences known to exist between innovators and their biosimilars is a great concern to physicians, particularly those treating complex and not completely understood diseases like cancer. Regulators will need to improve their communication and education in this area if biosimilar uptake is to increase.
The Roundtable concluded with agreement that continued dialogue between all stakeholders will be key. The concerns raised by physicians in Spain need to be heard and addressed if biosimilar uptake is to increase.
Speaker faculty
Professor Francisco José de Abajo, MD, MPH, PhD, Spain
Kevin Klein, MSc, The Netherlands
Sol Ruiz, PhD, Spain (Co-Chair)
Robin Thorpe, PhD, FRCPath, UK
Professor Francisco Zaragozá, PhD, Spain (Chair)
Interactive discussion session panel members
Professor Joan Albanell, MD, Spain
Olga Delgado Sanchez, PharmD, Spain
José Vicente Moreno-Muelas, MD, Spain
Professor Maria Jesús Sanz Ferrando, PhD, Spain
The Generics and Biosimilars Initiative (GaBI) wishes to thank Professor Francisco Zaragozá for his strong support through the offering of advice and information during the preparation of this Roundtable meeting.
The authors wish to thank Dr Beatrice Perks, GaBI Journal Editor, in preparing this meeting report and providing English editing support for finalizing this manuscript.
Competing interests: The Roundtable meeting was sponsored by an unrestricted educational grant to GaBI from Amgen Inc.
Provenance and peer review: Not commissioned; internally peer reviewed.
Professor Francisco José de Abajo, MD, MPH, PhD
Professor Joan Albanell, MD
Olga Delgado Sanchez, PharmD
Kevin Klein, MSc
José Vicente Moreno-Muelas, MD
Sol Ruiz, PhD
Professor Maria Jesús Sanz Ferrando, PhD
Robin Thorpe, PhD, FRCPath
Professor Francisco Zaragozá, PhD
References
1. GaBI Online – Generics and Biosimilars Initiative. Biosimilars approved in Europe [www.gabionline.net]. Mol, Belgium: Pro Pharma Communications International; [cited 2017 Feb 25]. www.gabionline.net/Biosimilars/General/Biosimilars-approved-in-Europe
2. European Medicines Agency. Guideline on good pharmacovigilance practices (GVP) Product – or Population-Specific Considerations II: Biological medicinal products. EMA/168402/2014. 4 August 2016 [homepage on the Internet]. [cited 2017 Feb 25]. Available from: http://www.ema.europa.eu/docs/en_GB/document_library/Scientific_guideline/2016/08/WC500211728.pdf
3. Abad Hernández MA, Andreu JL, Caracuel Ruiz MA. Position paper from the Spanish Society of Rheumatology on biosimilar drugs. Reumatol Clin. 2015;11(5):269-78.
4. Annese V, Avendaño-Solá C, Breedveld F, Ekman N, Giezen TJ, Gomollón F, et al. Roundtable on biosimilars with European regulators and medical v, Brussels, Belgium, 12 January 2016. Generics and Biosimilars Initiative Journal (GaBI Journal). 2016;5(2):74-83. doi:10.5639/gabij.2016.0502.019
|
Author for correspondence: Robin Thorpe, PhD, FRCPath, Deputy Editor-in-Chief, GaBI Journal |
Disclosure of Conflict of Interest Statement is available upon request.
Copyright © 2017 Pro Pharma Communications International
Permission granted to reproduce for personal and non-commercial use only. All other reproduction, copy or reprinting of all or part of any ‘Content’ found on this website is strictly prohibited without the prior consent of the publisher. Contact the publisher to obtain permission before redistributing.
Source URL: https://gabi-journal.net/roundtable-on-biosimilars-pharmacovigilance-traceability-immunogenicity-15-november-2016-madrid-spain.html
|
Abstract: |
Submitted: 4 June 2016; Revised: 7 September 2016; Accepted: 15 September 2016; Published online first: 28 September 2016
This interactive workshop was held on 2–3 March 2016 at the Hacettepe University in Ankara, Turkey using an almost identical format to what was used in prior educational workshops as reported in GaBI Journal. For more details of methods and case presentations, see the published report of the First Latin American educational workshop on similar biotherapeutic products [1] and the First MENA educational workshop on regulation and approval of similar biotherapeutic products/biosimilars [2].
The workshop was organized in collaboration with the Faculty of Pharmacy, Hacettepe University. Presentations were made by both international speakers as well as local academic faculty, clinicians and Turkish regulators. After the formal presentations (as done in the prior two workshops referenced above), the audience was presented with data for two semi-fictional follow-on biotherapeutic products, one a recombinant human erythropoietin (EPO) and the other a monoclonal anti-TNF antibody. The audience was divided into groups; each of which was asked to discuss specific questions about the potential approval of one of the two proteins under the direction of two to three local, university faculty and regulatory experts. The list of speakers and the slides they presented and the slides used to summarize the quality and clinical trial performance of the two products, are all available on the GaBI Journal website (www.gabi-journal.net/about-gabi/educational-workshops).
Summaries of parallel working group discussions are presented below.
Groups 1 and 2, who were assigned to evaluate the EPO product, chose to work together rather than separately. The specific questions they were asked and an edited simplified summary of their responses are presented in Table 1.
General summary information of Group 1 and 2 discussions is presented in Table 2.
EPO is one of the important glycosylated therapeutic proteins. Glycosylation patterns have effects on immunogenicity and half-life of therapeutic proteins by influencing the active clearance of a protein. Glycosylation is dependent on the number of sialic acid residues attached to the protein molecules. Glycans and sialic acids have effects on receptor binding and serum half-life. Serum half-life of the therapeutic proteins increase when the number of sialic acid residues increases. Glycosylation increases blood half-life but decreases receptor binding.
After manufacturing changes such as manufacturing site and method, the influence of in vitro potency activity should be evaluated. As sialic acid content and lactosamine extension is increased, serum half-life of the product is extended but receptor-binding affinity is decreased. Although the pharmacokinetic profile of the product could be estimated since the serum half-life of the product is known; potency values in patients could not be presumed because of the small differences which have an effect on receptor binding. Some bioassay parameters such as receptor binding and cell proliferation studies should be evaluated for estimating potency values in patients. Sialic acid content differences may increase potency values. Thus, increasing the degree of sialylation and glycosylation decreases the renal clearance rate and can increase EPO in vivo activity.
The structural characteristics of the therapeutic product such as glycosylation and product or process related impurities have effects on quality and immunogenicity of the protein product. Clinical immunogenicity is a key factor to determining safety and efficacy of biosimilars. It is important to note that only clinical studies are appropriate for detecting immunogenicity and for evaluation of clinical safety, at least 12 months of human immunogenicity data should be obtained.
The three groups who evaluated the IgG1 anti-TNF monoclonal antibody SBP candidate did so separately. The specific questions they were asked followed by the edited, simplified summaries of their individual group responses are presented in Table 3.
Group 4 included further summary information, see Table 4.
Despite the large and growing number of products being approved and marketed worldwide as ‘biosimilars’, there continues to be a lack of consensus concerning the best practices for the evaluation, approval, use and post-marketing surveillance of follow-on biologicals. While there were areas of general agreement in the case evaluations done by the participants in this workshop, there were many differences in participants’ responses and opinions from the participants concerning whether these two fictitious follow-on biologicals were qualified to be called biosimilars. This has also been seen in GaBI’s similar workshops.
These differences are likely a reflection of the fact that this is a relatively new area of pharmaceutical science and both the number of products and the information becoming available about the proper definition, approval, monitoring, substitution and switching of follow-on biological products are increasing rapidly. The lack of consensus suggests that academics and regulators, as well as prescribers and patients, need to be provided with the training and unbiased information needed for them to properly approve or regulate, prescribe, or use follow-on biological products, i.e. biosimilars.
Speakers
Dr Elwyn Griffiths, DSc, PhD, UK
Professor Dr Ibrahim C Haznedaroğlu, Turkey
Dr Sundar Ramanan, PhD, USA
Dr James S Robertson, PhD, UK
Dr Robin Thorpe, PhD, FRCPath, UK (Chair)
Dr Meenu Wadhwa, PhD, UK
Çisem Başak Budak, Turkey
Professor Philip D Walson, MD, USA/Germany (Co-Chair)
Dr Aydan Eratalay, PharmD, PhD
Bilgen Beldüz, MSc
Dr İsmail Burak Bal
Professor Dr Nazan Bergişadi, PhD
Fikriye Handan Çelikel, MSc
Assistant Professor Dr Devrim Demir Dora, PharmD, PhD
Professor Dr Türkan Eldem, Dr Nat Sci
Professor Dr R Neslihan Gürsoy, PhD
Dr Enes Karabulut, MD
Professor Dr Nefise Ozlen Şahin, PhD
Professor Dr Semra Şardaş
Professor Dr Sevda Şenel, MSc, PhD
Gökçe Yildirim
Assistant Professor Dr Devrim Demir Dora of Faculty of Pharmacy/Department of Pharmaceutical Biotechnology at Hacettepe University and Dr Aydan Eratalay from the Turkish Medicines and Medical Devices Agency had read the report, provided the discussion/conclusion of Group 1 and 2 and revised content of Table 2.
Professor Dr Sevda Şenel of Faculty of Pharmacy/Department of Pharmaceutical Technology at Hacettepe University had reviewed Group 3 discussions detailed in Table 3, and confirms that the summary reflects perfectly what has been discussed and decided.
Professor Dr R Neslihan Gürsoy of Faculty of Pharmacy at Hacettepe University had read Group 4 report detailed in Table 3, and commented that it was well prepared.
Professor Dr Türkan Eldem of Faculty of Pharmacy/Department of Pharmaceutical Biotechnology at Hacettepe University had reviewed Group 5 discussions detailed in Table 3 and made a few updates.
The Generics and Biosimilars Initiative (GaBI) wishes to thank Professors Bülent Gümüşel and Neslihan Gürsoy of the Hacettepe University for their strong support through the offering of advice and information towards the development and preparation of this interactive workshop.
The authors would like to acknowledge the help of all the workshop speaker faculty and participants, each of whom contributed to the success of the workshop and the content of this report, as well as the support of the moderators and co-moderators: Dr Aydan Eratalay, Bilgen Beldüz, Dr İsmail Burak Bal, Professor Dr Nazan Bergişadi, Fikriye Handan Çelikel, Assistant Professor Dr Devrim Demir Dora, Professor Dr Türkan Eldem, Professor Dr R Neslihan Gürsoy, Dr Enes Karabulut, Professor Dr Nefise Ozlen Şahin, Professor Dr Semra Şardaş, Professor Dr Sevda Şenel, Gökçe Yildirim, in facilitating meaningful discussion during the parallel case study working session, presented the discussion findings at the workshop and contributed in the finalization of this Meeting Report.
Competing interests: The workshop was sponsored by an unrestricted educational grant to GaBI from Amgen Inc.
Provenance and peer review: Commissioned; internally peer reviewed.
Robin Thorpe, PhD, FRCPath
Deputy Editor-in-Chief, GaBI Journal
References
1. Walson PD, Thorpe R. First Latin American educational workshop on similar biotherapeutic products, Mexico City, Mexico, 20 January 2015. Generics and Biosimilars Initiative Journal (GaBI Journal). 2015;4(3):143-8. doi:10.5639/gabij.2015.0403.031
2. Walson PD, Thorpe R. First MENA educational workshop on regulation and approval of similar biotherapeutic products/biosimilars, Dubai, United Arab Emirates, 1 September 2015. Generics and Biosimilars Initiative Journal (GaBI Journal). 2015;4(4):173-7. doi:10.5639/gabij.2015.0404.039
| Author for correspondence: Professor Philip D Walson, MD, Editor-in-Chief, GaBI Journal |
Disclosure of Conflict of Interest Statement is available upon request.
Copyright © 2016 Pro Pharma Communications International
Permission granted to reproduce for personal and non-commercial use only. All other reproduction, copy or reprinting of all or part of any ‘Content’ found on this website is strictly prohibited without the prior consent of the publisher. Contact the publisher to obtain permission before redistributing.
Source URL: https://gabi-journal.net/first-turkish-interactive-workshop-on-regulation-and-approval-of-similar-biotherapeutic-productsbiosimilars-2-3-march-2016-ankara-turkey.html
Author byline as per print journal: Vito Annese, MD, PhD; Cristina Avendaño-Solá, MD, PhD; Professor Ferdinand Breedveld, MD; Niklas Ekman, PhD; Thijs J Giezen, MSc, PharmD, PhD; Professor Fernando Gomollón, MD, PhD; Research Professor Pekka Kurki, MD, PhD; Professor Tore Kristian Kvien, MD; Professor Andrea Laslop, MD; Professor Lluís Puig, MD, PhD; Robin Thorpe, PhD, FRCPath; Martina Weise, MD; Elena Wolff-Holz, MD
|
Introduction: Biological drugs are improving therapeutic options for many diseases, but access to these therapies is being held back by costs. Biosimilars offer a lower-cost alternative to the corresponding original therapeutic protein, the reference product, with a comparable quality, safety and efficacy. Despite these apparent advantages, arriving at the best solution for patients will need improved communication between regulators and caregivers. |
Submitted: 24 January 2016; Revised: 21 April 2016; Accepted: 21 April 2016; Published online first: 4 May 2016
Access to biological therapies, despite their clear potential for the treatment of many diseases, is more or less restricted owing to high cost. The problem is likely to continue or even aggravate, as a growing number of biological therapies enter the market. It remains unclear whether healthcare systems will be able to make these therapies widely available. Stakeholders hope that biosimilars will have a significant impact on the sustainability of future pharmacotherapy. Regulators and learned societies, especially medical societies, have prominent roles in guiding the rational use of new medicines, including biosimilars.
European regulators and medical societies were the first to encounter biosimilars, and countries worldwide are looking to Europe for guidance.
The Generics and Biosimilars Initiative (GaBI), with its mission to foster the worldwide efficient use of high quality and safe medicines at an affordable price, organized a roundtable discussion for European regulators and medical societies on biosimilars with the aim of promoting interaction and sharing information in this increasing important area. It is important to respect the expertise and role of each stakeholder in the biosimilar discussion, agree Research Professor and former Chair of the European Medicines Agency’s (EMA) Biosimilar Medicinal Products Working Party (BMWP), Pekka Kurki of the Finnish Medicines Agency, Fimea, and Chair of the Roundtable on Biosimilars, and Dr Robin Thorpe, Deputy Editor-in-Chief of the GaBI Journal, expert of BMWP, formerly Head of Biotherapeutics Group of the UK’s National Institute of Biological Standards and Control and Co-Chair of the Roundtable.
On 12 January 2016, GaBI held a Roundtable on Biosimilars in Brussels, Belgium, with participation by European regulators and medical societies. The programme offered speaker presentations and parallel discussion groups to provide participants with important and up-to-date information related to many aspects of biosimilars with a focus on the key issues of comparability, extrapolation, interchangeability and substitution, as well as pharmacovigilance. Presentations were in English. The speakers were regulators but not official delegates of any regulatory body.
Differences between regulatory decisions and the recommendations of medical societies
The Roundtable was opened by the Chair, Professor Pekka Kurki, expert of BMWP, with an overview of European Medical Societies’ position papers on biosimilars, see Table 1. Restricting the overview to recent papers that were written in English, he focussed on the concerns and contrasting views contained within these papers with regards to the regulatory decisions. With the growth in biological therapies and the numbers of diseases they treat, there is a steadily growing number of position papers.

Overall, Professor Kurki noted that these papers were generally in favour of biosimilars, particularly for new patients. But there were mixed opinions on extrapolation, traceability, interchangeability and automatic substitution. Prescribing by brand name was favoured, and there were concerns over immunogenicity.
The biggest problem for physicians, and therefore for medical societies, is that biosimilars can never be exact copies of their reference products. This was a point made throughout the Roundtable in spite of the fact that minor variation of the physicochemical properties of different versions of the same product is an inherent property of all biologicals. Physicians across the board do not find this straightforward to explain to patients. The problem is particularly evident in a naturally relapsing/remitting disease like rheumatoid arthritis (RA). A patient who starts taking a biosimilar and suffers a relapse of symptoms may well blame the symptoms on the biosimilar, and doctors might not always be confident explaining that this is unlikely – given the comparability studies to which each biosimilar will have been subject.
Professor Kurki noted that it is important to recognize that biosimilars have a proven similarity without being identical to the reference product. According to medical societies, even sophisticated comparability testing, in vitro assays and animal studies cannot fully predict the biological and clinical activity of a therapeutic monoclonal antibody.
According to some position papers, extrapolation of indications approved for the originator drug to completely different diseases and age groups that are not based on adequate preclinical, safety and efficacy data (ideally phase I and phase III trials) should not be performed. In their view, extrapolation from rheumatoid arthritis and ankylosing spondylitis studies to Crohn’s disease (CD) and/or ulcerative colitis (UC) cannot be done unless information on mucosal healing, corticosteroid-free remission or immunogenicity and loss of response in CD or UC patients is provided.
The same concerns apply to paediatric patients. Studies specifically looking at outcomes such as growth and development are welcomed by some medical societies.
One concern shared by all the position papers reviewed by Professor Kurki’s team, was that of physician autonomy. It was important for all medical societies that their physicians could make their own therapeutic choices. ‘That is understandable, and we support that. But there are economic realities, and the question is how to apply prescribing autonomy in the best way for the benefit to patients and healthcare systems,’ says Professor Kurki.
Professor Kurki showed a figure illustrating the difference in development philosophies between biosimilars and the reference product, see Figure 1. Two pyramids (representing biosimilars on the left, and originators on the right) represent the marketing authorization documentation. The pyramid representing biosimilars starts at the base with quality documentation (pharmaceutical documentation), followed by an extensive portion dedicated to comparative in vitro studies, analytical, functional and structural testing side-by-side, and then a limited set of clinical trials, and at the top, the risk management plan (RMP). This is clearly different for the development of a new active substance, he notes. While both pyramids share the pharmaceutical documentation, with standards exactly the same for biosimilars as for new biologicals, the originator also has to investigate the pharmacology, the mode of action and the toxicology of the product. For biosimilars, those are already known. Then there is an extensive set of studies for absorption, distribution, metabolism, elimination and pharmacodynamics (PDs). For biosimilars, it is sufficient to demonstrate a comparable exposure after single or repeated administration. In the case of a new biological, every claimed indication needs to be studied, alongside special groups such as children or patients with organ dysfunction. Finally, as with biosimilars, the RMP needs to be in place.
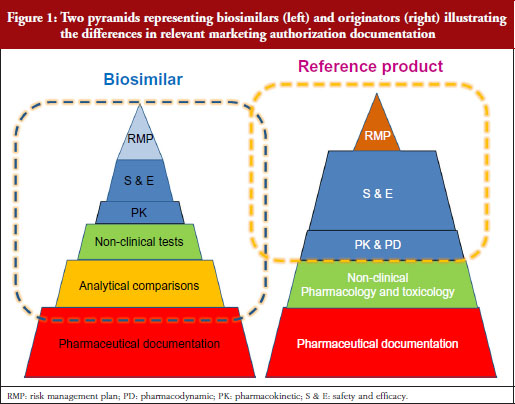
Our problem, suggests Professor Kurki, is that while the regulators look at the analytical and non-clinical testing and the clinical trials as one package (‘totality of evidence’) when deciding what is a biosimilar, clinicians focus on the clinical part only. This would explain, he suggests, the lack of confidence in comparability, while regulators seem more comfortable because they have been carrying out these studies for over two decades for manufacturing changes. This was discussed in more detail by Dr Niklas Ekman, also of Fimea.
Clinical biosimilar safety and efficacy studies look like typical phase III studies, but they are not; they have special features, e.g. looking at population pharmacokinetics (PKs) or PDs markers. Physicians see the active substance of biosimilar as new active substance, whereas regulators see it as a different version of the same active substance.
For specialists, it is difficult to accept that studies performed in one disease can be applied to another disease with different pathogenic features. Regulators, meanwhile, are more focussed on receptor binding and functional tests of the biosimilar, i.e. the mode of action of the active substance.
Manufacturing and characterization of biologicals
Dr Niklas Ekman, a member of EMA’s BMWP, explained how manufacturing process changes are common for all biologicals, both originators and biosimilars. He pointed to earlier studies showing the number of changes made to the manufacturing process of individual products since their approval [1], see Figure 2, and how manufacturing changes impacted on the glycosylation profile and antibody-dependant cell cytotoxicity (ADCC) of biopharmaceuticals – biopharmaceuticals that, from a physician’s point of view, would have been identical [2]. In other words, after a change in manufacturing process, originator biologicals are also not identical to earlier versions of the same originator biological. The comparability concept and its fundamental importance for the maintenance of safety and efficacy have remained unknown to physicians which may explain their reservations to biosimilars.
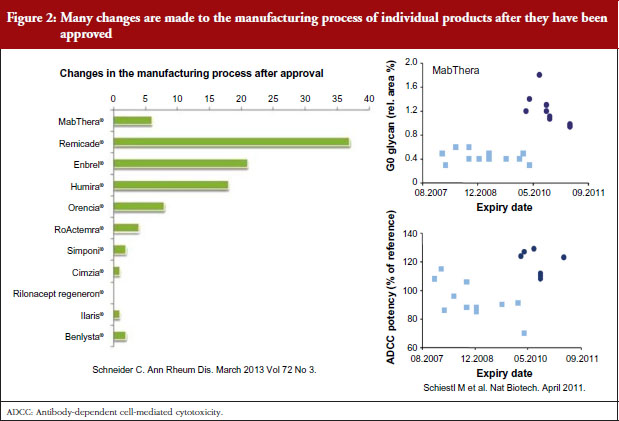
Clinical and non-clinical comparability
Professor Andrea Laslop of the Austrian Medicines Agency and a member of the EMA’s Committee for Medicinal Products for Human Use (CHMP), discussed clinical and non-clinical comparability for biologicals/biosimilars. The non-clinical development is based on the 3Rs: Reduce, Refine and Replace, animal studies as much as possible with in vitro data.
Comparability programmes at the clinical level can and must be strengthened by a number of factors, Professor Laslop urged. Comparability testing must use a homogeneous/sensitive population, a sensitive dose (or two doses), an appropriate model and statistical approach, and must use an accurate definition of the equivalence margin. The primary outcome measures need not be the same as those in the originator’s pivotal clinical trials. Orphan drugs raise unique challenges related to small population sizes. These challenges can be resolved in collaboration with regulatory authorities. Importantly, international dialogue between regulators is needed in order to encourage harmonization of regulatory requirements on a global scale. The final goal, says Professor Laslop, is to provide faster access for patients to affordable biological medicines at a sustainable price.
Immunogenicity
Dr Robin Thorpe, a member of EMA’s BMWP, focussed on the issue of immunogenicity. The European Union was the first to put together a guideline on immunogenicity assessment, he noted, and there is a revised version of this guideline due later in 2016. Immunogenicity issues occur all along the life cycle of a product, and particularly when a new therapeutic protein is developed and used for various clinical indications; when a change in process, formulation, or storage conditions is introduced or – notably given the topic of this roundtable – when a biosimilar product is proposed. Assessment requires an optimal antibody testing strategy alongside validated methodologies and reference standards. A better quality such as decreased immunogenicity does not preclude biosimilarity but needs to be justified as it possibly indicates a difference between products.
Extrapolation
Dr Martina Weise of the Federal Institute for Drugs and Medical Devices in Germany and Vice Chair of EMA’s BMWP discussed the principles of extrapolation of indications. Despite being the most contentious issue of biosimilar development, Dr Weise says extrapolation of indications is the single greatest benefit of biosimilar development.
Noting the data presented by Dr Niklas Ekman, see Figure 2, Dr Weise pointed out that extrapolation of data is already an established scientific and regulatory principle that has been exercised for many years, for example, in the case of changes in manufacturing process of originator biologicals. In such cases, clinical data are not required. In the development of biosimilars, clinical data are typically generated in one indication and, taking into account the overall information gained from the comparability exercise, may then be extrapolated to the other indications.
Dr Weise has recently published a paper on the science of extrapolation [3], with her regulatory colleagues, where the authors say they are not aware of any case of a change in the manufacturing process where more than one clinical study was required to compare two versions of the same product and this was sufficient for all approved indications.
Extrapolation must always be appropriately justified, and, where doubt remains, additional functional or clinical data are required for extrapolation to be granted. Dr Weise reminded delegates that scientific evidence and explanation of the reasons for extrapolation granted by CHMP may be found in the European Public Assessment Reports (EPARs).
Interchangeability
Dr Elena Wolff-Holz of Germany’s Federal Agency for Vaccines and Biomedicines, and a memberof EMA’s BMWP, discussed the interchangeability and substitution of biosimilars. She presented findings from a series of small to medium-sized switching studies involving biologicals and biosimilars, none of which showed any safety/efficacy signals that would justify extensive, longer studies.
For example, a Swedish study that investigated switching between the originator and biosimilar of the growth hormone (somatropin) showed no impact on patients’ growth velocity after switching to the biosimilar, see Figure 3 [4]. When a model was used to compare observed versus predicted growth, the predicted levels lay close to the observed data, showing excellent fit. Similar findings were shown for epoetin alfa-containing biosimilars, biosimilar filgrastim, biosimilar insulin glargine, and biosimilar infliximab. She also emphasized the value of EPARs (European Public Assessment Reports) in which results of biosimilars development programmes (epoetin, filgrastim, insulin glargine, somatropin), which included crossover trials with originators, are presented.
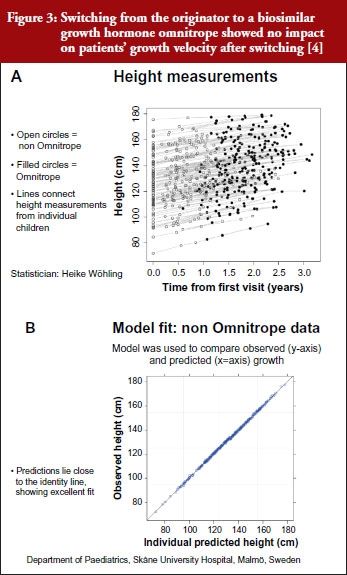
Referring back to the point made by Dr Niklas Ekman, see Figure 2, Dr Wolff-Holz reminded participants of the number of post-marketing changes made to biological drugs, notably monoclonal antibodies, without the need for further clinical studies. The regulators recalled only one case where clinical data were requested. The risk of rare adverse effects is best addressed by the RMP, as with any other medicinal product, she concluded.
Pharmacovigilance
Dr Thijs J Giezen, a hospital pharmacist at the Foundation Pharmacy for Hospitals in Haarlem, The Netherlands, and a member of EMA’s BMWP, discussed the safety assessment and risk management of biosimilars. Safety assessment is of paramount importance for biosimilars, with a particular focus on immunogenicity. Major differences in immunogenicity might question biosimilarity, he noted. As with all drugs, pharmacovigilance for originators and biosimilars is vital, and traceability is of specific importance.
When drawing up a pharmacovigilance plan for a biosimilar, post-marketing studies that not only compare safety profiles but also warn against rare adverse events are in a key position. Additional immunogenicity studies may be considered, perhaps in the context of studies that are already underway, for example, rheumatology registries, or – at a company’s own discretion – initiating new studies.
Physicochemical and functional comparability
It was asked whether the quality attributes of a biosimilar and its reference product will be compared in the same way as in the PK bioequivalence studies. It was clarified that, for the key quality attributes, the acceptable range is defined by the analysis of variability between batches of the reference product. For other quality attributes, the acceptable range depends on the type of analytical method. Therefore, statistical analyses are difficult to apply. The products are tested side-by-side to reduce variability. If differences are found, they will be judged by prior knowledge of previous analyses of different versions of proteins in the same class, analysing additional batches, and by using orthogonal methods to look at the same characteristics.
Impact of physicochemical and functional differences on safety and efficacy
Analytical comparability leans on the experience gained from studies of different versions of the active substance after a change of the manufacturing process. These changes are very common because the manufacturing processes need to be optimized, their scale is increased and manufacturing sites changed. Some participants were surprised by the variation between different versions of original biological products that have been accepted without clinical data. It was discussed whether clinical data should be requested more often before accepting a manufacturing change. The regulators responded that there is no evidence from clinical trials performed after licensing, such as expansion of therapeutic indications, that the safety or efficacy of current biotechnology-derived proteins would have changed over time significantly. The explanation is that analytical tests are more sensitive than clinical trials for showing differences.
The demonstration of comparability of monoclonal antibodies is challenging because they have several possible modes of action. Binding to the antigen is necessary for function but Fc-mediated functions may have a role as well. Nevertheless, all functions can be measured by in vitro analytical and functional tests. In the discussion, interpretation of these tests, especially the test for antibody-dependent cell-mediated cytotoxicity (ADCC) was discussed. The audience was concerned about the differences that have been demonstrated after manufacturing changes as well as differences between biosimilars and their reference products. In general, the role of Fc-mediated functions in the therapeutic effect is incompletely known. It was argued that it cannot be excluded that observed ADCC differences (~20%) have an impact on the efficacy or safety. Regulators responded that the differences often disappear when different effector and target cells are used or non-relevant antibodies are present. Sometimes the difference appears only in cells that have Fc-receptors with high affinity genotype. Glycosylation patterns that increase ADCC activity may have a clinical impact. Obinutuzumab is an anti-CD20 antibody that was glyco-engineered in order to enhance the binding to FcγRIIIa. As a result, its ADCC activity against different B-cell lines is 5- to 100-fold higher than that of the ‘wild type’ antibody. This antibody has been shown to be more effective than rituximab in depleting malignant B-cells in chronic lymphocytic leukaemia. Against this background, the small difference in the ADCC between the first biosimilar infliximab and its reference product appears insignificant, especially when considering the applied ADCC test using a target cell line that has been genetically modified to be very sensitive for anti-tumour necrosis factor (anti-TNF) effects.
Interestingly, serious problems after manufacturing changes have been associated with the drug formulation rather than the active substance itself. Pure red cell aplasia (PRCA) has been triggered initially by factors in drug formulation but not with the epoetin alfa itself.
Does comparability mean therapeutic equivalence?
It was asked whether there are examples of seemingly perfect analytical comparability but observed clinical differences at the same time or later. More than 200 cases of PRCA were observed in patients treated with the marketed original epoetin alfa after a manufacturing change. Likewise, decreased efficacy and increased reactogenicity have been observed after manufacturing changes of a few vaccines. So far, such differences have not been observed with biosimilars after licensing. One case of PRCA was detected in a clinical trial with a biosimilar epoetin alfa in development. The development was discontinued. Thus, the experience from the reference product and the extensive comparability exercise will help to identify possible problems already in the development phase of a biosimilar.
Can a biosimilar be better than its reference product?
A product cannot be biosimilar if it has inferior safety or efficacy. However, what if the product is superior? A biosimilar may have an improved quality profile, e.g. purity and immunogenicity. Reduced immunogenicity may lead to slower loss of efficacy and, thus, better adherence to therapy by some patients. Thus, the applicant has to justify the difference with regard to safety and efficacy. Increased efficacy is not possible for a biosimilar since it would make it impossible to refer to the documentation of the reference product which is the basis of the abbreviated development. According to the EU legislation, a ‘biobetter’ must be licensed as a new active substance.
Immunogenicity
It was pointed out that, in the future, there will be several biosimilars for the same reference product. This may lead to multiple switches for the same patient over time. Multiple switches are often said to increase the risks of immunogenicity. Should this scenario be tested before licensing of a biosimilar? Regulators responded that immunogenicity of each biosimilar and its reference product will be compared before licensing. For the time being, data from switching biosimilars and the reference product are reassuring. The current view among European regulators is that, once comparable immunogenicity has been demonstrated against the reference product, there is no need to perform specific switching studies.
Extrapolation
How to select the patient population for a clinical efficacy and safety study when the product is used in different diseases and patient populations using different combinations with other products that may interfere with the performance of the tested active substance was also discussed. It was also asked whether all combinations and diseases and dosing regimens should be tested. Regulators clarified that clinical safety and efficacy studies were preceded by PK and PD studies. The developer should not proceed to large clinical trials if comparability is not demonstrated. The safety and efficacy studies should be done in a clinical model that is representative for other models, i.e. therapeutic indications and populations, and which is sensitive for showing differences. The purpose of the safety and efficacy studies is to complement and confirm the comparability demonstrated at the previous steps of development. This approach requires that the clinical endpoints are sensitive to differences. Thus, the primary clinical endpoints selected for demonstration of comparable efficacy are not necessarily the same as those used in the pivotal clinical trials of the reference product at the time of licensing. For example, overall survival rate and time to progression are generally used in oncology to study a product with a new active substance. These endpoints are time related and usually take rather long time for evaluation. Therefore, a more reasonable and sensitive endpoint, such as overall response rate, may be used. Thus, testing in all therapeutic indications, populations and drug combinations is neither necessary nor feasible.
Disagreements on extrapolation
The concern about extrapolation by clinicians is the use of the same biosimilar or a new innovative product, notably monoclonal antibodies, in different diseases in which the mechanism of action is thought to be different. Infliximab, for example, used in rheumatology is thought to act predominantly through the neutralization of soluble and trans-membrane TNFα, whereas in other conditions such as Crohn’s disease, signalling through membrane-associated forms of TNFα and Fcγ receptors that may trigger apoptosis or ADCC may play a more important role.
Regulators responded by pointing out that the different functions of a therapeutic monoclonal antibody are always investigated by in vitro receptor-binding and cell-based functional assays. These assays are more sensitive than clinical trials. Therefore, regulators feel more comfortable than clinicians with the extrapolation of safety and efficacy between different therapeutic indications.
Clinicians pointed out that clinical experience from less formal, e.g. open label, studies will and have already relieved some concerns about extrapolation.
Clinicians are puzzled by the fact that, in case of the first biosimilar infliximab, Canadian regulators, in contrast to their European colleagues, did not accept the extrapolation of safety and efficacy from RA to inflammatory bowel disease (IBD). Does the fact that all therapeutic indications of the reference product were granted in the EU and later by the US Food and Drug Administration (FDA) mean that the future biosimilar infliximabs, or even etanercepts, will get all therapeutic indications of the reference product automatically? The current regulatory view is that the extrapolation is considered on the basis of the comparability exercise of a given product together with the justification by the applicant. Thus, it is a case-by-case decision.
Regulators’ expectation is that biosimilars approved in the EU will have the same therapeutic indications as the reference product. This is desirable from the pharmacovigilance point of view since a restricted set of therapeutic indications may lead to off-label use. Sometimes, the applicant is not seeking for all therapeutic indications because of patents or because of the lack of suitable, e.g. paediatric, formulation.
Off-target effects and biosimilarity
In general, it is a constant feature of clinical science to observe results that were not expected on the basis of previous knowledge. This is, indeed, almost always the situation after licensing of a product containing a new active substance. It was discussed whether unexpected off-target effects could be observed with biosimilars.
The regulators argued that biologicals, by their nature, have less off-target effects than chemicals. The long experience with the reference products helps to understand the effects of the active substance. A biosimilar will have the same effects, both beneficial and adverse, as the reference product. For biosimilars, the issue is whether new, unexpected off-target effects could be encountered in spite of the extensive comparability exercise. The discussion led to the topic of whether a comparable receptor interaction is sufficient to predict similar functional effects or whether differences in the downstream signalling pathways in target cells could be significantly different after the binding of the biosimilar and the reference product in spite of comparable results in functional cell-based tests, e.g. phagocytosis, apoptosis, ADCC. Regulators maintained that it is essential to separate the effects of the product from the responses of different types of target cells that may respond differently to the same signal. In the end, no agreement was reached on the significance of off-target effects with the use of biosimilars.
A possible off-target effect was mentioned in the context of cancer therapy and bone marrow after treatment with biosimilar filgrastim. Reference was made to the study of Brito et al. (Support Care Cancer. 2016; 24(2):597-603) in early breast cancer receiving (neo)adjuvant docetaxel/doxorubicin/cyclophosphamide therapy and prophylaxis with biosimilar, pegfilgrastim or reference filgrastim. The treatments were administered at different consecutive time periods and data were gathered retrospectively. The rate of febrile neutropenia (FN) per patient and treatment cycle was the same in biosimilar and reference filgrastim groups. The rate of FN and severe neutropenia (ANC < 100 cells/μL) was seen in 50% of patients in the biosimilar group but only in 4% in the reference product group. The authors concluded that ‘No differences in biosimilar effectiveness were detected. The clinical relevance of the profound neutropenia found in the biosimilar cohort needs further attention’. Interestingly, no such difference was found in the multicentre, double-blind, therapeutic equivalence study of biosimilar G-CSF versus the reference product in subjects receiving doxorubicin and docetaxel as combination therapy for breast cancer.
Interchangeability
There is some concern in the rheumatology community about the long delay of full publication of the safety results of the long-term extension of the pivotal safety and efficacy studies of the first biosimilar infliximab, especially the study in ankylosing spondylitis (PLANETAS). During the extension, ankylosing spondylitis patients were switched from the reference product to the biosimilar. The switched patients had a higher rate of adverse events and more withdrawals from the therapy. These results have been reviewed by the EU regulators who did not react to the difference, probably because of the relatively small number of patients at the time of the switch and lack of a plausible explanation. A publication featuring the safety data after the switch is pending.
It was pointed out that neither regulators nor prescribers across the Atlantic have a uniform opinion of the interchangeability. This is partly due to different regulatory frameworks in the two areas and partly due to the interpretation of the theoretical basis and available data.
In the EU, interchangeability is within the mandate of the Member States whereas in the US, interchangeability studies are mandatory by legislation. Interestingly, FDA has not published any guidance on how to study interchangeability. This may reflect the scientific problems related to the switching studies.
Pharmacovigilance
It is evident that the root cause of some adverse effects of biologicals, notably immunogenicity, is in the improper handling and storage of biologicals. It is particularly important to maintain the cold chain. This is becoming a challenge also in Europe when the administration and storage of biological medicines is more and more often taking place at home by the patient or caregiver. Innovative auto injectors and packages may mitigate this problem in the future for biologicals, including biosimilars.
The Roundtable ended with three parallel discussion groups, each of which included representatives from regulatory authorities and from medical societies. Groups were asked to discuss physicians’ attitudes to and concerns surrounding biosimilars – comparability, immunogenicity, extrapolation, interchangeability and substitution, as well as pharmacovigilance. Focus discussion topics included the thought process in preparing position papers, the bottlenecks, e.g. training, and the concerns and challenges faced.
Group 1 Summary
Summarized by Professor Fernando Gomollón, MD, PhD; presented by Professor Ferdinand Breedveld, MD
Group 1 identified a remaining doubt among clinicians, which could be reflected in the question: do in vitro tests really predict the appropriateness of extrapolation? After recognizing that this mere concept can be difficult to accept for clinicians, the general agreement of the group was that if a multiple set of well standardized tests, enough data on exposure in a sensible population and previous clinical data are all considered, extrapolation can be seen as a good concept, a real change of paradigm.
Some issues were raised about safety signals in PLANETAS data. For some people, safety data may require more clarification, although the general opinion was that if EMA had considered the signals as non-significant, they were probably not important.
Registries
There was general agreement among group members on the importance of registries. Ideally these should function on a national scale with a core of data that is easy to share between countries. More work on the definition of these registries is clearly needed.
A real philosophical (or pathophysiological, if preferred) question was also raised. Would a knowledge of the exact mechanism of action of a drug in a given disease make it easier to extrapolate? Perhaps in theory, but with the mechanisms of these diseases being so complex, the general agreement is that the EMA road to extrapolation is adequate in the current state of knowledge.
Good research, poor communication
Some open discussion was undertaken on the low opinion that clinical gastroenterologists have for biosimilars (although it seems rather clear that things are changing and opinions improving). The general agreement was that EMA has done really good scientific work with biosimilars, but not communicated their findings effectively. So, communications should be improved and coordinated, with contributions from EMA, scientific societies and other authorities.
Improving patient care
The group found two concepts that needed emphasizing: 1) biosimilars are not easy to approve in Europe; 2) to date, after approval, the safety record of biosimilars in Europe is really quite good (if not excellent).
Finally, the group agreed that cost is the main drive for biosimilars introduction. This should be seen as an opportunity for better patient care, and that negotiation between payers, authorities, clinicians, pharmacists and patients is the best way to implement change.
Group 2 Summary
Summarized by Cristina Avendaño-Solá, MD, PhD; presented by Vito Annese, MD, PhD
In a group that included four regulators, two rheumatologists, two gastroenterologists, one haematologist and one clinical pharmacologist, there was full agreement on the opportunity that biosimilars provide both in increasing accessibility to biological medicines and in decreasing costs. Those costs can then be diverted to other health spending. Cost benefits are, however, more likely to be related to the arrival of competition, which will drive down the price of the originator drugs. Another possible bonus of biosimilars is seen in preliminary data suggesting that biosimilars could be improvements on originators. They might have less impurities, reduced immunogenicity, or be administered by improved devices.
Switching
One concern shared by the group was how to introduce biosimilars in clinical practice. It is difficult to promote switching between originators and biosimilars in a chronically ill patient who is already taking the originator.
There is still some reluctance about the comparability exercise based on a limited number of parameters and limited clinical data. Recognition of the contribution of data post-authorization and the importance of pharmacovigilance are key.
Concerns were raised about interchangeability. There were doubts related to the absence of data and the potential impact of switching on individual patients. It is complicated to demonstrate interchangeability.
There were also concerns about multiple switching and how to preserve pharmacovigilance and immunogenicity monitoring of each specific product.
Benefits of cost cutting
The group recommended increasing the visibility of the usefulness of the money saved through biosimilars. For example, the agreement of using biosimilars in IBD could go hand-in-hand with actions such as providing extra nurses, support to registers and support for therapeutic drug monitoring (TDM). It is important to recognize the value of TDM to guide switching.
Group members recommended revising how systems of price and reimbursement decisions work at the country level. Involving patients in decision-making will increase their awareness of the benefits of biosimilars.
Group 3 Summary
Summarized and presented by Professor Lluís Puig, MD, PhD
Group 3 focused on monoclonal antibodies for the treatment of immune-mediated inflammatory diseases (IMIDs).
The question was raised whether biosimilars will remove inequity of access to expensive drugs. Group members agreed that access should not depend on price. The UK’s National Institute for Health and Care Excellence (NICE) is working to facilitate entry of biosimilars into the market, but faces many obstacles and concerns among patients and clinicians who are dealing with the unknown.
Switching
The group recognized opposition to switching in patients who are doing well. The only reason for them to switch would be cost, and the group discussed the importance of cost, budgeting and patients’ say. Problems arise around the issue of enforced switching without patients’ consent and full knowledge of safety, or physicians’ choice. The pressure is clearly on the physician. In oncology and haematology there is particularly low acceptance of switching.
The question was raised whether switching trials are needed. Available results show no significant change, but perhaps they are unlikely to do so given their design and power limitations.
In Denmark, there is a 69% discount on Remsima, and authorities enforced wholesale switching. Wholesale switching was similarly promoted in Austria.
NOR-switch is a study funded by the Norwegian Government, aimed to compare the originator infliximab (Remicade) and Celltrion’s biosimilar infliximab (Remsima) as regards disease worsening rates across all indications after one year of treatment. Thirty per cent is the expected worsening rate of Remicade, 15% the non-inferiority margin, and 500 patients are the population enrolled.
Safety
The issue of safety monitoring and the need for registries was discussed. The group raised doubts on quality of monitoring, and asked who will pay for it. In most countries it is unrealistic that governments will pay for monitoring.
In the UK, NICE made a formal requirement that prescribers included new patients treated with biosimilars into registries. There is a need for tracking. There is a need to collect the data regardless of how likely it will be to see a result. There are huge methodological challenges with registries.
Extrapolation
The group looked at real-life data from the Czech Republic showing no difference between originators and their biosimilars. The same was shown for paediatric indications. Regulators do not care so much about the disease in which the trials are being made.
There is a very large difference in perception and acceptance between individual countries. In the Czech Republic, physicians today have no objection to switching and extrapolation based on their results. The situation has changed in 2015, based on education and experience.
Biosimilarity exercise
The group discussed how subjects for clinical trials of biosimilars cannot be found in Western Europe; they have early access to potent therapy and do not progress to levels of activity making them eligible for enrolment. Furthermore, the ethics of a clinical trial that does not provide a clinical advantage was discussed.
There was a concern that PK studies in healthy volunteers may not be representative for all indications in which PK may vary. The regulatory view is that the variability in patients is more dependent on confounding factors than on the active substances.
A request was made for further detail or transparency in preclinical data. An understanding of the way regulatory agencies make their decisions is needed, rather than calling for ever-increasing numbers of clinical trials.
It was concluded that biosimilars have the potential to increase patients’ access to biological therapy. Clinicians keep asking for more data and tailored information, especially on the safety and practical conduct of the switches between the biosimilar and its reference product. There is a consensus on the need for a better traceability and surveillance of adverse events of all biologicals. Physicians would like to see data of biosimilars in new or established registries.
Information and transparency are the key issues. It is not only data, as information is available, but only scarce information that is tailored towards different groups of stakeholders. Prescribers, maybe even different specialities, need different information, patients, hospital pharmacists and maybe payers as well. This is one of the take home messages – not only for regulators. Regulators will certainly give a signal to agencies and EMA that the emphasis on information should be even more than it is today.
This information should not only be tailored to the different stakeholders, it also should be focused on certain issues. Information available on several interesting factors can be put together as needed for each stakeholder. One of the issues that has been raised is whether physicians can explain the comparability exercise, especially the physicochemical in vitro biological aspect, and how decision-making is based on those tests.
Prescribers need information on extrapolation, they need to explain why therapeutic indications have been granted without clinical trials. This is another message that delegates at the Roundtable will need to bring back to their organizations and agencies.
The structure–function relationship, what can be said from individual results of analysis, how it can be concluded that a difference in an analytical test is not important, all needs to be explained to patients.
The Chair added one particular target for information, namely extrapolation of safety and efficacy. There are not enough regulators to explain to all stakeholders what extrapolation is, what analytical testing is, and so on. This has to be a collaborative exercise. The information received from London or from Brussels, prepared by multi-disciplinary multi-national teams, is very complicated. This information needs to be tailored according to national healthcare providers and society in general.
Physicians at the meeting were of the opinion that the information on the whole development cascade has helped to put the difficult issues, such as extrapolation and interchangeability, into a clearer context. Yet the limited data on the difficult topics, especially on interchangeability, is still of concern.
The presentation on the physicochemical and structural as well as in vitro functional analyses as the basis for comparability of different versions of both the original and biosimilar products and the long experience of these studies helped clinicians understand the concept of biosimilarity. The fact that the original biological products are not, from a physicochemical point of view, the same as at the time of licensing – because they have been subject to many manufacturing changes over their life cycle – was surprising to some delegates. One delegate even went on to say that it was a shame that physicians had not been aware of the manufacturing process change data shown by Dr Niklas Ekman and others, see Figure 2, which might have made switching to biosimilars less worrying. Any differences in a drug are feared, but it is now clear that physicians have been prescribing non-identical versions of the same drug for years.
Perhaps not surprisingly, the group discussions all agreed that the position of the physician is a difficult one when switching patients from the original product to the biosimilar. Physicians must keep up to date with the latest data in this area, and are personally accountable to their patients for their treatment decisions. On one hand, clinicians do not have the possibility to judge all data that were available for regulators at the time of marketing authorization. On the other hand, positive experience from some members of the groups reduced the level of uncertainty and anxiety.
It is not easy for a physician who has had success with an originator drug to switch to a biosimilar for cost reasons. It may be difficult to persuade a patient to switching to an alternative drug because it is cheaper, rather than because it is better. The health service overall stands to gain through cost savings, not the individual patient. Therefore, switching plans should incorporate some extra values for the patients, increasing their awareness of the benefits of biosimilars.
In at least two discussion groups, it became clear that Czech physicians are relatively unconcerned by switching. This was attributed to a successful education campaign, and to not being under cost pressures. Physicians from other countries often described how they felt they were being put under pressure to make cost savings from which they and their patients would not directly benefit. Perhaps learning about biosimilars and what they are, before being put under pressure to cut costs, would have made switching easier to deal with.
Conflict of interest was mentioned in the discussions. Biosimilarity is an area with high commercial interest. The regulators have extremely stringent rules for conflict of interest. Such rules are not possible in the clinic because it would be very difficult to run clinical trials. Nevertheless, relationships with industry should be somehow managed in order to maintain credibility. This is an issue that both regulators and prescribers need to be very much aware of.
The post-marketing follow-up is another area where physicians and regulators have common interests, especially how to make the most of registries. Current registries have been useful but there have been clear drawbacks; they are not available in every country, the ones that exist are useful for certain purposes but they are not compatible with each other, and it can be difficult to get information by pooling the data from different registries.
The national agencies should consider ways to contribute to registries. There are economic issues; who will fund the registries, how will the people who maintain it be reimbursed? This is also a political issue, since people are sensitive with their information/personal data and hence, permission from the patient is needed to use the data. This is an area where collaboration is required, including a strong signal from clinicians and regulators that these data are important for health care and for individual patients.
Traceability was discussed in the context of having several biosimilars, price competition and tendering processes. This situation may lead to multiple switches that should be documented. TDM was considered slightly outside the typical regulatory scope. There is some information in the summary of product characteristics if the company has been able to provide the necessary information. However, usually this is not the case and TDM is more for academics and clinicians who develop these systems.
Costs were not included in the presentations of this meeting although there is no other incentive to use biosimilars than lower price/costs. Physicians may have to change their role in the biosimilar discussion. The positive consequences of the price competition that is triggered by biosimilars needs to be understood. Roundtable Chair Professor Pekka Kurki hoped that delegates did not mind this kind of remark: ‘Economics are there and times will not improve, it will be harder in the future,’ he said. Instead of maintaining a very conservative attitude, there is another option to become active and try to get the best out of this situation, he said. ‘Think what you can do to induce cost savings with your prescription behaviour. There are examples, from the Czech Republic and the UK, as to how biosimilars can help save money that can be used for other purposes.’
The Roundtable Chair concluded that the pleasant and constructive atmosphere of the meeting supported fruitful discussions, and testified for the importance of dialogue between regulators and physicians. Dialogue increases the mutual trust that is needed when new products and concepts are introduced to health care. The story of biosimilars is not yet at its end, this meeting was an interim analysis. Stakeholders need to be vigilant as the story unfolds.
It appears that the information on biosimilars has not been sufficient to satisfy the needs of prescribers. Physicians were interested in the way physicochemical, structural analyses and in vitro functional tests are used to demonstrate comparability and in the definition of acceptable differences. EPARs contain valuable information on biosimilars. However, their value for clinicians would increase if the crucial decisions such as extrapolation would be better justified. The European regulatory network, EMA and national regulatory agencies, need to find solutions to fill the obvious information gap.
Most of the position papers of medical societies were quite conservative and some contained requirements that would make the development of biosimilars unfeasible. It is evident that prescribers and regulators have different understanding of the biosimilar concept. The situation is changing since more information has become available and since experience from countries that have introduced biosimilars in massive scale, including switches, has been reassuring.
As a consequence, biosimilars are seen more often as an opportunity than a threat. A new situation is emerging in which regulators and prescribers can collaborate in planning managed switches and in tailoring information to various stakeholders, patients, pharmacists, payers. Pharmacovigilance was recognized as an important field of collaboration. Adverse effect reporting of biologicals, including the batch numbers, should be intensified. Collaboration between and within healthcare centres and hospitals as well as pharmacies is necessary to ensure traceability and early detection of rare adverse effects. Regulatory authorities may be able to promote the use of registries in monitoring the use of biosimilars.
Prescribers are in an uncomfortable situation when planning switches in individual patients who will not get immediate benefit and who may have concerns in using biosimilars instead of the original product. Payers and hospital administration should consider granting some incentives to healthcare units that will introduce biosimilars to their patients, e.g. the possibility to use the saved money to improve patient care by introducing new therapies.
Closing the meeting, Co-Chair Robin Thorpe explained that an event like this could only be the first step to reaching a consensus. The strength of such a Roundtable format allowed stakeholders from different and sometimes opposing camps – physicians (rheumatologists, gastroenterologists, dermatologists, haematologists, oncologists), pharmacists and regulators – to discuss their principles and concerns openly. Any conclusions from the event can only reflect what was agreed at the meeting, and what was not agreed.
Speakers
Niklas Ekman, PhD, Finland
Thijs J Giezen, MSc, PharmD, PhD, The Netherlands
Research Professor Pekka Kurki, MD, PhD, Finland (Chair)
Professor Andrea Laslop, MD, Austria
Robin Thorpe, PhD, FRCPath, UK (Co-Chair)
Martina Weise, MD, Germany
Elena Wolff-Holz, MD, Germany
Moderators and Co-moderators
Vito Annese, MD, PhD, Italy
Cristina Avendaño-Solá, MD, PhD, Spain
Professor Ferdinand Breedveld, MD, The Netherlands
Professor Fernando Gomollón, MD, PhD, Spain
Professor Tore Kristian Kvien, MD, Norway
Professor Lluís Puig, MD, PhD, Spain
Participants
Miguel Angel Abad Hernandez, MD, Spain, Spanish Society of Rheumatology (SER)
Vito Annese, MD, PhD, Italy, Italian Group for the Study of IBD (IG-IBD)
Professor Federico Argüelles-Arias, MD, PhD, Spain, Spanish Society of Gastroenterology (SEPD)
Cristina Avendaño-Solá, MD, PhD, Spain, Spanish Society of Clinical Pharmacology (SEFC)
Professor Jürgen Braun, MD, Germany, German Society for Rheumatology (DGRh)
Professor Ferdinand Breedveld, MD, The Netherlands, European League Against Rheumatism (EULAR)
Professor Antonio Costanzo, MD, Italy, Italian Society of Dermatology (SIDeMaST)
Professor Maurizio Cutolo, MD, Italy, European League Against Rheumatism (EULAR)
Assistant Professor Marc Ferrante, MD, PhD, Belgium, European Crohn’s and Colitis Organisation (ECCO)
Professor Fernando Gomollón, MD, PhD, Spain, European Crohn’s and Colitis Organisation (ECCO)
Professor Dr Richard Greil, MD, Austria, Austrian Society of Hematology and Medical Oncology (OeGHO)
Barney Hawthorne, DM, UK, British Society of Gastroenterology (BSG)
Ana Hidalgo-Simon, MD, PhD, UK, European Medicines Agency (EMA)
Professor Tore Kristian Kvien, MD, Norway, European League Against Rheumatism (EULAR)
Professor Milan Lukáš, MD, PhD, Czech Republic, Czech Society of Gastroenterology (CSG)
Professor Alexander MacGregor, MD, PhD, UK, British Society for Rheumatology (BSR)
Professor Massimo Massaia, MD, Italy, Italian Society of Experimental Hematology (IESS)
Associate Professor Dan Nordström, MD, PhD, Finland, Finnish Society of Rheumatology (FSR)
Marieke Pereboom, PharmD, The Netherlands
Bea Perks, PhD, UK
Professor Roberto Perricone, MD, Italy, Italian Society for Rheumatology (SIR)
Laura Pirilä, MD, Finland, Finnish Society of Rheumatology (FSR)
Professor Lluís Puig, MD, PhD, Spain, European Academy of Dermatology and Venereology (EADV)
Riccardo Saccardi, MD, Italy, Italian Group for Bone Marrow Transplantation (GITMO)
Professor Maria-Jesús Sanz Ferrando, PhD, PharmD, Spain, Spanish Society of Pharmacology (SEF)
Lasia Tang, BSc, MBA, Belgium
Apologies
Gonzalo Calvo, MD, PhD, Spain, European Association of Clinical Pharmacology and Therapeutics (EACPT)
Professor Marco Matucci Cerinic, MD, PhD, FRCP, honfbsr, Italy, Italian Society for Rheumatology (SIR)
Professor Silvio Danese, MD, PhD, Italy, European Crohn’s and Colitis Organisation (ECCO)
Professor João Eurico Cortez Cabral da Fonseca, MD, PhD, Portugal, Portuguese Society of Rheumatology (PSR)
Professor Maurizio Vecchi, MD, Italy, Italian Group for the Study of IBD (IG-IBD)
The Generics and Biosimilars Initiative (GaBI) wishes to thank Research Professor Pekka Kurki for his strong support through the offering of advice and information during the preparation of this Roundtable meeting.
The authors would like to acknowledge the help of all the roundtable speaker faculty and participants, each of whom contributed to the success of the meeting and the content of this report as well as the support of the moderators: Dr Vito Annese, Dr Cristina Avendaño-Solá, Professor Ferdinand Breedveld, Professor Fernando Gomollón, Professor Tore Kristian Kvien and Professor Lluís Puig, in facilitating meaningful discussion during the parallel group discussions, and presented the discussion findings at the meeting.
The authors wish to thank Dr Bea Perks, GaBI Journal Editor, in preparing this meeting report manuscript and providing English editing support on the group summaries and for finalizing this manuscript.
The PLANETAS and PLANETRA extension studies including full safety data have been published online in Annals of Rheumatic Diseases after the meeting of Roundtable on biosimilars with European regulators and medical societies: Park W, et al. Efficacy and safety of switching from reference infliximab to CT-P13 compared with maintenance of CT-P13 in ankylosing spondylitis: 102-week data from the PLANETAS extension study. Ann Rheum Dis. 2016;0:1-9. doi:10.1136/annrheumdis-2015-208783
Yoo DH, et al. Efficacy and safety of CT-P13 (biosimilar infliximab) in patients with rheumatoid arthritis: comparison between switching from reference infliximab to CT-P13 and continuing CT-P13 in the PLANETRA extension study. Ann Rheum Dis 2016;0:1-9. doi:10.1136/annrheumdis-2015-208786
Competing interests: The Roundtable meeting was sponsored by an unrestricted educational grant to GaBI from Hospira UK Ltd.
Provenance and peer review: Not commissioned; internally peer reviewed.
Vito Annese, MD, PhD
Cristina Avendaño-Solá, MD, PhD
Professor Ferdinand Breedveld, MD
Niklas Ekman, PhD
Thijs J Giezen, MSc, PharmD, PhD
Professor Fernando Gomollón, MD, PhD
Research Professor Pekka Kurki, MD, PhD
Professor Tore Kristian Kvien, MD
Professor Andrea Laslop, MD
Professor Lluís Puig, MD, PhD
Robin Thorpe, PhD, FRCPath
Martina Weise, MD
Elena Wolff-Holz, MD
References
1. Schneider CK. Biosimilars in rheumatology: the wind of change. Ann Rheum Dis. 2013 Mar;72(3):315-8.
2. Schiestl M, Stangler T, Torella C, Cepeljnik T, Toll H, Grau R. Acceptable changes in quality attributes of glycosylated biopharmaceuticals. Nat Biotechnol. 2011;29(4):310-2.
3. Weise M, et al. Biosimilars: the science of extrapolation. Blood. 2014;124(22):3191-6.
4. Flodmark CE, et al. Switching from originator to biosimilar human growth hormone using dialogue teamwork: single-center experience from Sweden. Biol Ther. 2013;3:35-43.
5. GaBI Online – Generics and Biosimilars Initiative. Norwegian study may be slowing adoption of biosimilar infliximab [www.gabionline.net]. Mol, Belgium: Pro Pharma Communications International; [cited 2016 Apr 21]. Available from: www.gabionline.net/Biosimilars/News/Norwegian-study-may-be-slowing-adoption-of-biosimilar-infliximab
|
Author for correspondence: Research Professor Pekka Kurki, MD, PhD, Finnish Medicines Agency, PO Box 55, FI-00034 Fimea, Finland |
Disclosure of Conflict of Interest Statement is available upon request.
Copyright © 2016 Pro Pharma Communications International
Permission granted to reproduce for personal and non-commercial use only. All other reproduction, copy or reprinting of all or part of any ‘Content’ found on this website is strictly prohibited without the prior consent of the publisher. Contact the publisher to obtain permission before redistributing.
Source URL: https://gabi-journal.net/roundtable-on-biosimilars-with-european-regulators-and-medical-societies-brussels-belgium-12-january-2016.html
Copyright ©2025 GaBI Journal unless otherwise noted.